INVOLVEMENT OF PRESURGICAL PAIN IN PREEMPTIVE ANALGESIA FOR ORTHOPEDIC LIMB SURGERY
Sumihisa Aida*. Koki Shimoji (SPON: K. Dan), Dept ofAnesthe-siology, Niigata Univ School of Medicine, Niigata, Japan
Aim of Investigation: To clarify our speculation that pain existing before surgery may induce central sensitization, thus making preemptive analgesia (PA) ineffective.
Methods: Patients undergoing limb surgery were allocated to PA or control groups. Pain was rated using a visual analogue scale. Some had presurgical pain (fracture surgery, and arthritis surgery), while others had no presurgical pain (removal of a limb tumor, nail or plate). For preemptive treatment, morphine (bolus 0.06 mg- kg-1-h-1 before surgery, and continuous 0.02 mg-kg-1-h-1 during surgery) was administered epidurally at the C6-7 (upper limb) or LI-2 (lower limb) level. After complete recovery from anesthesia, a patient controlled analgesia pump was set to inject epidural morphine.
Results: Pain (6-48 h after surgery) in patients undergoing surgery with PA was significantly lower (p<0.005) than those without PA. However, patients undergoing fracture or arthritis surgery with PA had no significant reduction in pain as compared to those undergoing the same surgery without PA. Patients undergoing surgery with PA used significantly less morphine (p<0.005) than those without PA. In fracture or arthritis surgery, however, there were no significant differences in morphine consumption between patients with PA and those without PA. There were significant correlations between pre- and postsurgical (6 h) VAS values in patients undergoing fracture and arthritis surgery with PA.
Conclusions: Central sensitization may be pre-established by presurgical pain, and the presurgically imprinted central sensitization is preserved until the termination of surgery. Presence of presurgical pain might be responsible for the controversy over the clinical validity of PA.
CAN PRE-EMPTIVE EPIDURAL ANALGESIA WITH SUFENTANIL REDUCE POSTOPERATIVE PAIN AFTER ABDOMINAL HYSTERECTOMY?
Ethem I. Akural, Timo E Salomaki, Seppo Alahuhta*, Dept of Anaesthesiology, Univ ofOulu
Aim of Investigation: To investigate the pre-emptive effects of epidural sufentanil administration before surgery and after the closure of the peritoneum during total abdominal hysterectomy.
Methods: Forty-four ASA physical status I or II patients undergoing elective total abdominal hysterectomy were studied in prospective, randomized, double-blind design. Epidural catheters were placed in the L1-L2 interspace. The study group received epidural sufentanil (50 ug in 20ml normal saline) before surgical incision, followed by epidural normal saline (20 ml) after the closure of the peritoneum. The control group received epidural normal saline (20 ml) before surgical incision, followed by epidural sufentanil (50 (ig in 20ml normal saline) after the closure of the peritoneum. No additional analgesics were used before or during the operation. Anesthesia was induced with propofol (2 mg/kg) and maintained with propofol infusion and isoflurane. The postoperative analgesia consisted of patient-controlled epidural sufentanil. Result: After exclusions, there were 20 patients in the study group and 21 in the control group. There were no difference in pain scores (Verbal Numeric Analog Scale) at rest and during mobilization. Expressed pain scores over 3 days confirmed correct use of the PCEA device and that those taking less sufentanil were not in more pain. The sufentanil consumption over 72h in both groups is demonstrated in table 1. early postoperative PCEA sufentanil consumption were similar in both groups, the study group used less analgesia in the 12 to 18 h period relative to the control group.
Conclusions: The results of the present study suggest that preemptive epidural sufentanil is associated with a short-term opioid-sparing effect, which is most pronounced between 12-18 and 36-42 hours.
Table 1 Sufentanil Consumption via patient control epidural analgesia over time intervals. Data are median (interquartile range) sufentanil consumption (ug). (Mann-Whitney U test)
| Study group | Control group | 95 % Cl of difference | P | |
| 0-6 h | 48 (39-77) | 52 (32-66) | -14,5to21,5 | 0,695 |
| 6-12 h | 30 (24-67) | 56 (34-84) | -36 to 4 | 0,097 |
| 12-18 h | 24(16-60) | 48 (36-76) | -32 to -4 | 0,022 |
| 18-24h | 40 (25-83) | 60 (48-84) | -36 to 4 | 0,123 |
| 24-30 h | 24(16-54) | 44 (20-50) | -20 to 8 | 0,346 |
| 30-36 h | 20(12-28) | 28(12-34) | -12 to 8 | 0,68 |
| 36-42 h | 16(8-23) | 22(12-28) | -12to0 | 0,114 |
| 42-48 h | 18(9-32) | 28(13-35) | -12to4 | 0,461 |
| 48-70 h | 72(40-110) | 74 (44-92) | -28 to 32 | 0,718 |
PREEMPTIVE ANALGESIA WITH BUPIVACAINE FOLLOWING INGUINAL HERNIA REPAIR.
R. Atcheson. P. Gill*, S. Kiani*, A. Victoria*. Univ Dept of Anaesthesia and Pain Management, Leicester Royal Infirmary, Leicester LEI 5WW, U.K.
Aim of Investigation: To determine ifbupivacaine can produce preemptive analgesia for inguinal hernia repair.
Methods: This double blind study recruited 40 patients planned to have an inguinal hernia repair under general anaesthesia. All patients received a field block with 40 ml of 0.375% bupivacaine. Patients were randomised (with sealed envelopes) to receive the block as follows: Group 1 (Pre): after induction of anaesthesia and 10 minutes before the start of surgery. Group 2 (post): at the completion of surgery and 10 minutes before the end of anaesthesia.
Results: There was no difference in the median pain scores at rest, coughing or sitting up in the six hours after surgery between the two groups. 24 hours after surgery there was a trend towards higher pain scores in the "post" group compared with the "pre" group and this was statistically significant (p<0.05) at rest (figure 1). Average daily pain scores on days 2 to 7 showed no difference between the two groups.
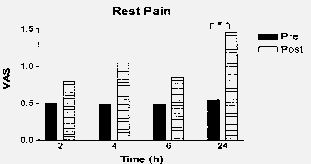
Figure 1. Median pain scores at rest in the 24 h after surgery. * significance <0.05.
Conclusions: A field block with bupivacaine induces preemptive analgesia following inguinal hernia repair. Previous studies have failed to demonstrate a pre-emptive effect with lignocaine. The results from the present study suggest that the duration of block may be an important factor in the induction of pre-emptive analgesia with local anaesthetics.
THE INFLUENCE OF PREEMPTIVE KETAMINE ON EPIDURAL AND PERIPHERAL BUPIVACAINE BLOCK IN SURGICAL PAEDIATR1C PATIENTS.
Annette Gross'*. Fabrice Montigaud*, Claude Dubray', Alain Es-chalier', Bernard Dalens*, Chirurgie Infantile, Hotel Dieu and 'Groupe NPPUA, Faculte de Medecine, CHU, 63001 Clermont-Ferrand, France
Aim of Investigation: To evaluate the influence of the addition of ketamine (K) to bupivacaine (B) on the duration of sensory block and analgesia during epidural (Ep) and peripheral (Pe) blocks in children.
Methods: After ethics committee approval and informed parental consent were obtained, 72 paediatric patients undergoing elective surgery under Ep (n=36, B: 1 mg/kg) or Pe (n=36, B: 0.5-0.75 mg/kg) blocks were studied. The patients in each group were randomly assigned to receive 1) K (0,5mg/kg) added to B plus subcutaneous (SC) placebo 2) B plus SC K (0,5mg/kg) or 3) B plus SC placebo. Duration of sensory blockade, adverse effects and time to first analgesic were noted. Plasma concentrations of K were measured 20 min after injection. Differences were assessed using the Kruskal-Wallis test.
Results: Motor blockade and adverse effects were similar in all groups. After Ep B local K prolonged the duration of sensory blockade (mean ± SD) (table). After Pe B this prolongation was of borderline significance. The time to first administration of analgesics in 50% of patients (FA50; median) was prolonged by local Ep K but not local Pe K. Even though SC K produced higher or similar K plasma concentrations than local K (mean ± SD), sensory block and analgesia were not prolonged after Ep or Pe B.
| Epidural B | Placebo | KSC | K Local | P |
| Duration:min FA50: min K: ng/mL Periphery B Duration:min FA50: min K: ng/mL |
220±84 259 272±165 503 |
266±119 267 131±51 264±119 375 141±56 |
366±U5 1135 86±37 407±190 521 82±43 |
0.02 0.01 0.01 0.06 0.80 0.10 |
Conclusions: Prolongation of B sensory block occurs after both Ep and Pe K, but not after SC K. This reinforcement is therefore locally, not systemically, mediated.
THE EFFECTS OF STOMACH CANCER SURGERY ON IMMUNOMODULATION AND NEUROENDOCRINE RESPONSE: COMPARISON OF ANESTHESIA AND ANALGESIA METHODS
Anthony TaeHyung Han. M.D.. SungKyunKwan Univ, College of Medicine, Samsung Medical Center, Pain Management Center, Seoul, 135-730. S.Korea
Aim of Investigation: Surgery causes alterations in immune and neuroendocrine responses. Cytoldnes, stress hormones and peri-operative medications like morphine could be important mediating factors which modulate the various immune responses. The aim of this study was to investigate 1) whether preemptive anesthesia and aggressive postoperative epidural analgesia and 2) the effect of different doses and amounts of morphine used for different postoperative analgesic techniques can have any effects on the concentrations ofproinflammatory cytokines and stress hormones in upper abdominal surgery.
Methods: Total 19 elective gastric cancer patients were randomly assigned in double blind fashion into two groups. Group-G(n=9) was provided with general anesthesia plus morphine intravenous patient controlled analgesia(IV-PCA), whereas Group-GE(n=10) with preemptive epidural and general anesthesia plus continuous postoperative epidural analgesia. Operating and anesthesia time, total morphine doses and complications were assessed. At predetermined time interval, proinflammatory cytokines and stress hormones and visual analog scales were evaluated. Results: Demographic data, the durations of operation, anesthesia, and recovery of GI function were similar in both groups. Total morphine doses were approximately four times greater in Group-G. Secretions of interleukin !/?, TNFcr and epinephrine were lessened by preemptive epidural anesthesia, meanwhile interleukin-6, ACTH and cortisol showed no such effect. 24 hours after skin incision, the differences of cytokines and stress hormones between two groups were disappeared. In spite of these findings, the visual analog scales could not disclose any differences. Incidences of complications were statistically insignificant except that of itching in Group-GE.
Conclusions: Preemptive epidural anesthesia and analgesia can partially prevent the release of some of the cytokines and stress hormones. These effects do not seem to have long term influences more than 24 hours. The amounts and/or ways of morphine administration by either IV-PCA or continuous epidural analgesia for postoperative pain control do not appear to have any effects on immunity at clinical dose range.
PREEMPTIVE ANALGESIA: COMBINATION OF MORPHINE, KETAMINE AND CLONIDINE IN HUMANS
H. Holthusen'. P. Backhaus2, F. Boeminghaus3, P. Lipfert', Zen-trum fur Anaesthesiologie', Heinrich-Heine-Universitat, Dussel-dorf; Kliniken far Anasthesie2 und Urologie3, Lukaskrankenhaus, Neuss, Germany
Aim of Investigation: To test whether a combination of three anti-nociceptive drugs with different site of action each (opioid-, NMDA-, ai-receptors) exerts substantial preemptive analgesia. Methods: 30 patients undergoing transperitoneal nephrectomy in general anaesthesia received (randomized, double-blind) ketamine, morphine (150 |^g/kg, each), and clonidine (5 u.g/kg) either before incision or immediately after wound closure. Statistics: median [range], Mann-Whitney U test
Results: No differences were found with respect to postoperative piritramide request by PCA pump (92 [22-210] mg vs. 93 [6-166] mg; p=0.65) or cumulative pain scores (20 [8-28] % Visual Analogue Scale vs. 21 [6-48] % VAS; p=0.53). (0% VAS=no pain, 100%=tolerance maximum).
Conclusion: Preemptive application ofopioids, NMDA-antago-nists, and aa-receptoragonists have separately been shown to attenuate post-traumatic sensitization in animals. In humans, however, even a combination of these drugs does not exert an apparer clinical useful protective effect. Thus, the attractive concept of preemptive analgesia appears not to be applicable to the clinic. Acknowledgments: Supported in part by the Rheinisch- West-falische Gesellschaft fur Urologie and Dr. Carl Thomae GmbH.
PREVENTION AND TREATMENT OF POST- OPERATIVE PAIN
N.A. Osipova. V.A. Beresnev*, N.A. Loseva*, Moscow Hertzen Cancer Research Inst, Russia
Aim of Investigation: To elaborate effective and safe methods of prophylaxis and post-operative (p/o) pain relief in patients undergoing different oncological operations. Methods: 522 oncological patients who underwent different surgery were examined. We used combinations of various central (CA) and peripheral (PA) analgesics for prophylaxis and p/o pain relief, such as NSAID (ketoprofen, diclofenac, ketorolac), antiki-ninogen (trasilol or others), opioids (morphine, promedol, prosidol, buprenorphin, tramadol, butorphanol). Quality of postoperative analgesia (POA) (VRS 0 to 4, cortisol and glucose blood plasma levels) and analgesics tolerability (frequency and severity of side effects on 0-3 scale) were estimated. In all cases the principle of "preemptive analgesia" was applied.
Results: Comparative analysis has revealed the most effective and tolerable components of POA. In moderate traumatic surgery (abdominal gisterectomy, laryngectomy with lymphadenectomy and others, 1st group n=47) the combination of NSAID (ketoprofen 100 mg/day i.m. 1 hour before surgery and 200-300 mg/day after surgery) with moderate potential opioid - tramadol in post operative dose 200-400 mg/day was enough for effective analgesia (VRS 0.38 +/- 0.23). In major abdominal operations (gastrectomy, hemi-colectomy and others, 2nd group n=315) good analgesia (VRS 0.4+/- 0.3) and normal cortisol (542.3 +/- 70.1 nmol/1) and glucose (5.2 +/- 0.7 mmol/1) plasma levels were obtained when two strong-action PA: NSAID (the foregoing schedule) and antikinino-gen (trasilol 500000 ME i.v. during operation and 300000 ME/day in p/o period) were used in combination with tramadol (400 mg/day p/o). In thoracal surgery prophylaxis and p/o pain relief were effectively achieved (VRS 0.3 +/- 0.2, levels of cortisol 532.0 +/- 78.6 nmol/1, glucose 5.0 +/- 0.3 mmol/1) with mentioned above two PA in combination with strong action opioid buprenorphin in dose 0.6-0.9 mg/day. Severe side effects and complications were not registered.
Conclusion: Combination of two strong-action PA - NSAID (ketoprofen or others) and antikininogen (trasilol or others) with one of the most safe opioids (tramadol, buprenorphin) in moderate doses was shown to be highly effective in prevention and treatment of p/o pain in major surgery.
PREEMPTIVE ANALGESIA WITH PETHIDINE IN PATIENTS AFTER CHOLECYSTECTOMY
Miroslava Pjevic, Clinical Center ofNovi Sad, Inst of Surgery, Dept of Anaesthesia and Intensive care, Hajduk Veljkova 1-9, 21000 Novi Sad, Yugoslavia
Aim of Investigation: To investigate whether pethidine administration before skin incision is more effective in reducing postoperative pain than the same drug given intraoperatively.
Methods: 30 patients (ASA 1 to 2) aged 40 to 65 years, scheduled for elective laparotomic cholecystectomy entered the study. Group 1 (n=15) received 1 mg/kg pethidine iv 5 minutes before induction of anaesthesia (before skin incision) and 0.9% NaCI of equal volume intraoperatively (after peritoneal opening). Group 2 (n=15) received pethidine and 0.9% NaCI in a reverse manner. Premedi-cation as well as other analgesics at induction and intraoperatively were omitted. Anaesthesia was induced with thiopentone and suc-cinylcholine for tracheal intubation. Pancuronium was administered for muscle relaxation and halothane with O^/N^O for maintenance of anaesthesia. The duration of surgery (time from skin incision to skin closure) and time from skin closure to the first analgesic request were recorded. All patients were sent to the ward after the first analgesic request and pain intensity estimation using VAS. Patients were given metamizol 2500 mg im at request during the first 12 h. If the regimen was not sufficient, piritramide 2 mg im was prescribed. The intensity of pain was estimated before the first analgesic request and 4, 8, 12 and 24 h thereafter. Data were presented as mean ± SD.
Results: Analyzing duration of surgery and time from skin closure to the first analgesic request (63.1±26.2 /60.0135.8 min; t=0.233) no significant difference was found between two investigated groups (p>0.05). The postoperative analgesic requirements were similar in both and no piritramide requirement was recorded. VAS scores at each examined time did not differ between the groups (p>0.05).
Conclusions: The results of the study proved no preemptive effect of pethidine. Preemptive administration of pethidine compared with the postinjury administration did not attenuate pain and analgesic consumption postoperative! y.
Acknowledgments: Supported in part by The Provincial Secret, of Health.
THE EFFICACY OF PRE-EMPTIVE MULTI-MODAL ANALGESIA ON PAIN AND OPIOID CONSUMPTION AFTER ANTERIOR CRUCIATE KNEE LIGAMENT REPAIR.
Ola Rosaeg. Barbara Krepski, Nicholas Cicutti, Dept ofAnesthesi-ology, Ottawa Hospital-Civic Campus, 1053 Carling Ave., Ottawa, ON K1Y4E9, Canada
Aim of Investigation: To compare opioid consumption and pain scores after anterior cruciate ligament (ACL) surgery with semi-tendinosis tendon graft in patients receiving multi-modal preemptive analgesia versus administering the same regimen after completion of the procedure.
Methods: 20 ASA 1 or II patients were randomized into 2 groups. Patients in Group I received: 1. Intra-articular injection with 20 ml ropivacaine 0.25% with 1:200,000 epinephrine and 2 mg morphine 2. ketorolac 30mg i.v. 3.. femoral nerve block with 20ml 0.25% ropivacaine. These drugs were given 15 minutes before skin incision. A standardized general anaesthetic, without i.v. opioids, was administered. Group II patients received the multi-modal analgesic combination immediately after the completion of surgery. I.V. PCA morphine was available for pain relief after surgery. Verbal pain scores (0-10) were recorded at specific time intervals after surgery and by telephone interview on post-operative days 1, 3 and 7.
Results: Interim analysis reveals that total post-operative morphine consumption was lower in Group I (6.6 ± 5.4 mg SD) vs Group II (13.7 ± 12.0 mg SD) P= 0.10. Similarly, verbal pain rating scores show a trend toward lower values in Group I at each time interval compared with Group II. Conclusions: Multi-modal pre-emptive analgesia for ACL knee surgery appears to decrease opioid consumption and pain after surgery. Final data analysis will be presented after completion of patient recruitment.
WHAT MAKES DIFFERENCES? PAINFUL HERPES ZOSTER V.S. PAINLESS HERPES ZOSTER
Hidetoshi Sato, Takehiko Makino*, Yukiko Noda*, Sumio Fuku-moto*, Kiyoshi Harano, Tadahide Totoki, Dept of Anesthesiology, Koseikan Saga, Prefectural Hospital, 1-12-9 Mizugae, Saga 840-8571 Japan and Dept of Anesthesiology & Critical Care, Saga Medical School, Japan
Aim of Investigation: Herpes Zoster (HZ) is one of the most common pain syndromes encountered in clinical practice. HZ usually presents with severe pain, paresthesia and multiple vesicle formation. Recently we had two cancer patients with painless HZ and intended to analyze these two cases.
Methods: Two cancer patients with painless HZ were investigated.
Results: [Case 1 ] A 60-year-old man with nasopharyngeal cancer and multiple lung metastasis were administered codeine phosphate 120mg/day and acetaminophen ISOOmg orally since March 26th, 1998. The patient was experiencing paresthesia and multiple vesicle formation on the rt. T4 area on May 6, 1998, but did not complain any pain. He died without any pain on May 30, 1998. [Case 2] A 48-year-old man with adrenal cancer and multiple liver metastasis was administered MS contine® 30mg/day, loxoprofen sodium 1 SOmg/day, alprazolam 1.2mg/day orally since September 11,1998. The patient was experiencing paresthesia and vesicle formation on the rt. T4 area on December 4,1998, but did not complain of any pain. He has had no pain since the onset of HZ.
Conclusions: Patients with HZ usually have severe pain during the acute stage. In 10-50% of patients with HZ, pain may prolong after healing of the vesicular lesions. However the above two patients had no pain both the onset and after healing of the vesicular lesions. Narcotics and anti-inflammatory drugs may work as preemptive analgesic agents.
COMPARISON OF ANALGESIC EFFECT OF PRE-OPERATIVELY USED PETHIDINE AND TENOXICAM
M. A. Sayan*, A.Yucel, S. Ozyalcin, G. K. Talu, S. Erdine. Dept. ofAlgology, Medical Faculty of Istanbul, Istanbul Univ. Capa 34390, Istanbul - Turkey
Aim: We aimed to compare the preoperative analgesic effect and side-effects ofiv pethidine (P) and iv tenoxicam (T).
Methods: With informed consent and approval of local ethical committee, 40 ASA I-II patients (18-65 years) who were scheduled for upper and lower abdominal surgery were randomized into two equal groups. Group T patients (11 male and 9 female) received 40 mgr tenoxicam (Tilcotil®, Roche) and Group P patients (8 male, 12 female) received 50 mgr pethidine preoperatively via iv route. A standard general anesthetic technique was used for all patients without use of non-steroid analgesic drugs and opioids. For postoperative analgesia all the patients received iv pethidine with patient controlled analgesia (Abbott, Pain Management Provider M). Pethidine delivery parameters were: 0.5 mgr/kg loading dose, 2 mgr/hr basal infusion rate, 5 mgr bolus dose and 15 minutes lockout time. The usual monitoring included: 48 hours opioid analgesic consumption. Visual Analogue Scale (VAS), sedation score (SS) (5 pt. scale), SpO-i, blood pressure (BP), heart rate (HR) in 1, 12, 24, and 48 hours. Plasma pethidine levels were measured in 24 and 48 hours. Data were statistically analysed.
Results: There were no differences in groups regarding sex, age, ASA, VAS and vital parameters. After surgeries total dose of opioid consumption in Group T (263.5±68.9 mgs) was found significantly (pO.001) lower than Group P (328.6 ± 64.1 mgs). Also plasma pethidine levels' of Group T at 24. (71.32±47.35 ng/ml) and 48 hour (26.89±19.32 ng/ml) were found significantly (p<0.05) lower than Group P at the corresponding hours (138.9U87.03 ng/ml and 56.65±34.98 ng/ml respectively). The incidence of side effects were found to be similar.
Conclusion: We have concluded that preoperative administration of tenoxicam reduces the postoperative pain and consequently the analgesic demand and also the plasma pethidine level.
PREVENTION OF PHANTOM LIMB PAIN THROUGH PREVENTION OF CORTICAL REORGANIZATION
Niels Birbaumer''3. Katja Wiech', Stephanie Topfher2, Elena Huse' 'Inst of Medical Psychology and Beh Neurobiology, Univ ofTue-bingen, D-72074 Tuebingen, Germany, ^ept ofAnesthesiology, Univ of Tuebingen, D-72074 Tuebingen, Germany Dept of Psychology, Univ ofPadova, 1-35131 Padova, Italy
Aim of Investigation: Previous studies by our group (Flor et al 1996, Birbaumer et al 1997) have demonstrated that phantom limb nain is ffliispri hv cnrtipal re.riri”ani7ation of SI. Conseauentlv. a peripheral and central blockade ofnociceptive input before, during and after amputation should prevent the development of phantom limb pain.
Methods: Magnetic source imaging is used to measure cortical reorganization in three groups of upper limb amputees before and several days and months after amputation: Group 1 receives me-mantine only before and after amputation, Group 2 receives me-mantine and brachial plexus anesthesia, Group 3 receives standard pain medication and central anesthesia. Changes in pain experience is measured with a standardized set of psychological and psycho-physical procedures (see Flor et al 1996).
Results: Preliminary results of several patients in each group are presented. These preliminary data indicate a strong effect ofme-mantine on the prevention of phantom limb pain. As expected, cortical reorganization is strongly related to the intensity of phantom pain: contralateral to the site of amputation the distance between the cortical representation between face and hand area at SI is reduced in pain patients, leading to an ..invasion" of the lip representation in the hand area.
Conclusions: Tentative conclusions may point toward an effective prevention of cortical reorganization and phantom pain by the in-activation of plastic intracortical NMDA-receptor-fibres. Acknowledgments: Supported by the Deutsche Forschungsgemein-schaft (DFG) and "Fortune" of the Medical Faculty of the Univ of Tuebingen
PREVENTION OF PAIN ON INJECTION WITH PROPOFOL. A QUANTITATIVE SYSTEMATIC REVIEW.
M. Tramer', P. Picard2. 'DAPIC, CH Cantonal, Geneva, Switzerland, consultation Douleur, Hopital Fontmaure, 63407 Chamalieres, France
Background: Pain on injection with propofol is a common problem. Different methods have been proposed to prevent this pain. Methods: Systematic search for RCTs comparing an analgesic intervention with placebo or no treatment to prevent pain on injection with propofol. The primary endpoint of interest was prevention of any pain. Dichotomous data ("no pain" with active and with control) were quantitatively analysed using relative risk (RR) and number-needed-to-treat (NNT) with 95% confidence intervals (CI). A fixed effect model was used to combine data. Results: 38 RCTs with data on 4,180 patients met our inclusion criteria. Interventions tested were heat, cold, NSAIDs, opioids, local anaesthetics, barbiturates, different solvents, tourniquet, speed of injection, and others. On average 72.8% (range 36.4% to 100%) of patients reported some degree of pain or discomfort on injection of propofol. Most frequent documented analgesic intervention was lignocaine. It was given intravenously before the injection of propofol with or without venous occlusion, or mixed with propofol. There was evidence for dose-responsiveness (Table).
|
|
Event rates ("no pain") | No patients without paln/ Total No patient | Relative risk | Number-needed-to-treat | ||
| Ligno | J2S . . Control | Ligno | Control | (95% CI) | (95% CI) | |
| Lignocaine, before | ||||||
| 10 | 42.3% | 30.9% | 121/286 | 87/282 | 1.37(1.10(01.71 | 8.7 (5.2 to 28) |
| 20 | 70,6% | 45.7% | 48/68 | 32/70 | 1.54 (1.15 to 2.08 | 4.0 (2.5 to 11) |
| Lignocaine, mixture | ||||||
| 5 | 25.4% | 14.9% | 45/177 | 26/175 | 1.71 (1.11 to 2.64 | 9.5 (5.3 to 44) |
| 10 | 45.2% | 19.9% | 161/356 | 74/372 | 2.27 (1.80 to 2,87 | 3.9(3.1 to 5.3) |
| 20 | 64.0% | 16.3% | 194/333 | 50/307 | 393(3.01 to 5.14 | 2.1 (1.8 to 2.4) |
| 30 | 28.8% | 10.7% | 15/52 | 6/56 | 2.69 (1.13 to 6.42 | 5.5 (3.0 to 29) |
| 40 | 59.6% | 19.5% | 65/109 | 22/113 | 3.06 (2.04 to 4.59 | 2,5 (1.9 to 3.5) |
| Lignocaine, before + occlusion | ||||||
| 20 | 76.1% | 15.3% | 54/71 | 11/72 | 4.98 (2.85 to 8.71 | 1,6 (1.4 to 2.1) |
| 40 | 92.9% | 29.5% | 39/42 | 13/44 | 3.14(1.98(05.00 | 1.6(1.3to2.1) |
Conclusions: Lignocaine prevents pain on injection with propofol. The optimal regimens seems to be 20 mg, mixed with propofol.
PREEMPTIVE MUTUAL ADMINISTRATION OF LAMOTRIGINE AND MGS04 DECREASES THE LEVEL OF POSTOPERATIVE PAIN AFTER SPINAL SURGERY
Yury Y. Kobeliatsky, MD, PhD. Dept ofAnesthesiology, State Medical Academy, Dnepropetrovsk, 320044, Ukraine Aim of Investigation: To evaluate the affectivity of mutual administration drugs with different mechanism of action for modulation excitatory process during postoperative period for pain relief improvement.
Methods: In patients after spinal surgery we used Lamictal (Lamo-trigine®, GlaxoWellcome) 50-lOOmg PO 2 days before operation (1 group.). MgS04 30mg/kg IV 5 min. before operation (2 group,). mutual administration (3 group), morphine on demand (control group) There were 10 patients in each group. After operation we investigated: 1) VAS (mm), 2) the time of first demand of morphine after operation (hours), 3) total morphine consumption in the first day (mg).
Results: We have found the lowest level of VAS in the 3 group (45±4, p<0.05) comparatively with 1,2,4 group (55±17, 52±12, 78±15). The time of first demand of morphine in 1,2, and 3 group was 3.5010.21, 4.30±0.14, 5.10±0.14 and statistically significant (p<0.05) compared with the 4 group (1.40±0.09, p<0.05). The total morphine consumption in the 3 group were the lowest between all other groups (p<0.005). As in the 1 as well as in the 2 group the quality of postoperative pain relief was much better than in the control group
Conclusions: Glutamate mechanisms play an important role in development and maintenance ofhyperalgesia and demand on modulation of excitatory mechanisms for its remover. The mutual administration oflamotrigine (prevention presinaptic glutamate uptake) and MgS04 (block ofNMDA receptor canal and prevent Ca^ influx) for management ofpostincisional pain has better results comparatively with traditional analgesia and use each of these drugs alone.
THE EFFECT OF INTRAARTICULAR MORPHINE AND CLONIDINE ON POSTOPERATIVE ANALGESIA AFTER KNEE SURGERY.
Pong Hee Kirn. Dept ofAnesthesiology, College of Medicine, Dankook Univ, Cheon An, Chung Nam 330-714, Korea
Aim of Investigation: Intraarticular injection ofbupivacaine, cloni-dine and morphine produce good postoperative analgesia. This study was designed to compare the analgesic effect ofintraarticular clonidine and morphine, used separately and in combination,
Methods: We studied 60 patients undergoing arthroscopic anterior cruciate ligament reconstruction of knee under spinal anesthesia using hyperbaric 0.5% bupivacaine. Each patient received 30 ml of intraarticular 0.25% bupivacaine containing clonidine 150 u.g (Group C: n=20) or morphine 2 mg (Group M: n=20) or both (Group CM: n=20) after operation. Pain was assessed on visual analogue scale (VAS) at 0, 1, 2, 6, 12,24, 36,48 hr after operation.
Results: There was no difference in VAS score and the dosage of postoperative analgesics among the three groups.
Conclusions: We concluded that 30 ml of 0.25% bupivacaine containing morphine 2 mg or clonidine 150 ug provided comparable analgesia after intraarticular administration, but the combination of these drugs did not seem to increase analgesia
9th WORLD CONGRESS ON PAIN, 1999, Vienna, Austria, p.580 - 584






