MANAGEMENT OF CHRONIC CANCER PAIN IN THE TUNISIAN PAIN CENTER
M. Abdelmoula. M. Maiek, D. Gharbi, I. Fennira, M. Haddad, Pain Center ofRabta, Tunis, Tunisia
Pain control should be a priority in cancer care. For most patients (pts), the basic strategies are direct and pharmacologic: up to 85% of cancer pain can be managed with oral agents.
Aim of Investigation: The aim of this retrospective study was to evaluate the recruitment of the Tunisian Pain Center between Nov 1996 and Nov 1998, and to compare the quality of management of cancer pain during this period.
Methods: In this study, we reviewed demographic data of patients, the extent and causes of pain, the use of methods for pain evaluation (type of pain, intensity), principles of pain management and side effects of pain treatment, and evaluation of the response to treatment.
Results: One hundred and twelve patients with chronic cancer pain were studied. Eighty-two males and 30 females, aged between 10 and 84 years old, with an average age = 57.8 years. The most frequent site of the primitive tumor was lung (20 pts); prostate (13 pts); pancreas (10 pts) bladder (9 pts); rectum (7 pts); colon (7 pts). Seventy-two pts had pain ofnociceptive type; 29 pts had mixed pain and 11 had neurogenic type. Pain was severe in 63% of pts. Opioid agents were used in 72% of pts. Only 70 pts were available for response to pain treatment. After treatment, pain decreased in 54% of pts and was absent in 17%. The pain was unchanged for 29% of pts.
Conclusion: With understanding the mechanisms of pain, the knowledge of opioid agents (use and prescription) and the treatment of their side effects, cancer pain will be controlled better than in 96. But physicians and nurses need more education in pain evaluation and pain treatments. Many improvements are still necessary.
ASSESMENT AND TREATMENT OF CANCER PAIN, IN BASIS TO EVIDENCE, FOLLOWING (WHO) WORLD HEALTH ORGANIZATION GUIDELINES.
Margarita Araujo. Sara Bistre, Pain Clinic, American British Cow-drey Medical Center, Mexico City, CP 01120 Mexico.
Aim of Investigation: Treat cancer pain following WHO guidelines and interventional management, to patients in the final stage in hospital or at home with basis for individual and adequate pain relief.
Methods: Assessment of 100 cancer pain patients. Establishing type and staging of the illness, relationship with age and sex. Classifying characteristics and pain intensity. Analgesic treatment depending mean pain, intensity with non-opioid, opioid analgesics was accompanied by adjuvants, psychotherapy, physiotherapy and interventional management. Evaluating duration and efficacy of relief pain, pre- and post-antineoplastic treatment and palliative care. Observing the cause and place of the final treatment.
Results: 79% of the group with the mixed pain. Bone pain of more intensity and frequency 65%. Visceral pain in Pancreas and Colon cancer of difficult control, because of frequency of intestinal obstruction. Treatment duration from one week- to three years. Pain relief: good 20%, satisfactory 65%, inadequate 11% and bad 4%. 16 patients continue to be controlled, 80 were attended until dead, 72 in the home and 8 in the hospital.
Conclusions: Relief pain is achieved in most of cancer patients, by applying analgesics according to the guidelines of the WHO, based on an individual response. Until the final stage, both in the hospital and their home. It is important that this management begins since the first evidence of pain caused by the disease or the antineoplas-tic treatment.
CANCER PAIN RELIEF ACCORDING TO THE WHO ANALGESIC LADDER IN A HOSPITAL BASED PALLIATIVE CARE UNIT
D. Beck*. G.G. Hanekop, D. Kettler*. Dept ofAnaesthesiology, Emergency-Medicine and Intensive Care, Georg-August Univer-sitat, Robert-Koch-Str. 40, 37075 Gottingen, Germany.
Aim of Investigation: To investigate the management of pain in a specialist palliative care unit according to WHO 3-step ladder approach. The frequency, way of changing step as well as necessity for application of additional invasive analgesic methods and efficacy of treatment were recorded.
Methods: A retrospective chart audit was performed to explore the characteristics of 175 consecutive cancer patients.
Results: During admission 42 (24%) patients had no analgesic medication, 9 (5,1%) were treated according to WHO step I, 5 (2,9%) according to step II und 119 (68%) according to step III. At the end of treatment only 12 (6,9%) patients needed no analgesic medication, 7 (4%) were treated according to step 1, 4 (2,3%) according to step 2 und 152 (86,9%) according to step 3. In 10 (5,7%) patients, invasive analgesic methods as spinal opioids or nerve blocks were necessary. Maintenance or change of WHO step were as follows:
| No Change of WHO step | Pat. (%) | |
| 139(79,4) | ||
| stepO | 12 (6,9) | |
| step 1 | 6 (3,4) | |
| step 2 | 2 (1,1) | |
| step 3 | 119(68,0) | |
| Change of WHO step | Pat. (%) | |
| 36 (20,5) | ||
| step 0 - | -” step 1 | 1 (0,6) |
| step 0 - | -> step 2 (directly) | 2 (1,1) |
| step 0 - | •> step 3 (step by step) | 9 (5,1) |
| step 0 - | + step 3 (directly) | 18 (10,2) |
| step 1 - | •* step 3 (directly) | 3 (1,7) |
| step 2 - | •” step 3 | 3 (1,7) |
Treatment of pain was successful in 77% of patients at the beginning compared to 85% at the end of palliative care.
Conclusion: Specialist palliative care units are dealing with highly selected patients who mostly get strong opioids already during admission. In nearly 20% of the remaining, changing to WHO step III was necessary, mostly in a direct way. In 6% invasive analgesic methods were inevitable.
USE OF COMPLEMENTARY THERAPIES TO MANAGE CANCER PAIN IN SOUTH AFRICA.
Susan L. Beck. Univ of Pretoria, Pretoria 0001 RSA and Univ of Utah, Salt Lake City, Utah 84112 USA
Aim of Investigation: To describe the use of complementary therapies for cancer pain in South Africa.
Methods: 426 cancer patients with pain in inpatient, outpatient, and home settings completed a questionnaire that included the Brief
Pain Inventory and a checklist of complementary therapies. The survey was translated into 6 of the 11 official languages.
Results: The sample included 194 (46.1%) whites and 232 (53.9%) people of color including blacks, coloreds, and Indians. Nearly one-third of the entire sample experienced pain of severe intensity and only 21% of patients reported 100% pain relief. 92.5% reported using at least one type of complementary therapy; 28% used five or more types. The most often used therapies were prayer (61.2%), positioning (43.5%), not thinking about it (31.5%), and television (28%). The least frequently used included ice (1.8%), plasters (1.3%), hypnosis (2.7%) and acupuncture (2.7%). More whites than non-whites used heat (35.1% vs. 19%), seeing a minister (38.1% vs. 22.1%) and positioning (56.2% vs. 32.3%). More non-whites used menthol (15.5% vs. 7.2%), herbs (10.6% vs. 1.5%) and singing (11.5% vs. 2.1 %). Participants identified 23 additional activities that they used for pain relief. The most frequent was talking to people (n=25).
Conclusions: Complementary therapies are widely used by patients with cancer pain in South Africa. Similar findings were reported in U.S. studies although most of these studies used an open-ended interview vs. a structured checklist. Across studies, a high percentage of patients reported using positioning, heat, and forms of distraction. More effective use of both pharmacologic and non-pharmacologic therapies is needed to improve pain management for the significant number of cancer patients with unrelieved pain in South Africa.
Acknowledgments: Fulbright Scholar Program, United States Information Agency.
FACTS, INSUFFICIENCIES AND CONTRADICTIONS IN ONCOLOGIC PAIN THERAPEUTICS
Correia D. Silva R, Freitas D*, Femandes F*, Alves E*, Centro Hospitalar do Funchal, Medeira Island, Portugal
Introduction: Pain is a major symptom in neoplastic illness, being frequently underevaluated, modifying and altering patients' life quality.
Aim of Investigation: The authors evaluated the efficiency of analgesic therapeutics prescribed to oncologic patients, in Hospital and Ambulatory, in Madeira Island.
Methods: The authors built up a questionnaire and tested its reliability (test/retest/reliability) and validity (contents, construction and validity criteria). They applied it to a population of 350 people of two professional groups (doctors and nurses) who are in contact with this pathology in the exercise of their profession.
Results: The authors have analyzed 300 questionnaires, evaluated and documented the most used antialgig therapeutics, its clinical efficiency, the use and the difficulties in prescribing these drugs.
Conclusion: the authors conclude that oncologic pain is often un-derconsidered, treated with insufficient and not protocoled therapeutics; they also observed significant differences between the two queried professional groups.
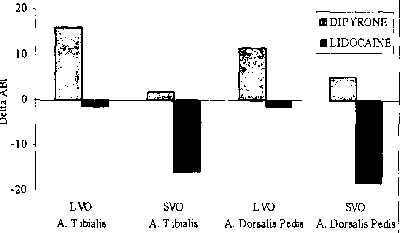
THE EFFECTS OF EPIDURAL DIPYRONE IN TERMINAL CANCER AND BURGER PATIENTS
M. Oral', M. Tulunay', SO Terzioglu', H. Ergun2, FC Tulunay2 of 'Anesthesiology & Reanimation and Pharmacology & Clinical Pharmacology, Univ of Ankara Faculty of Medicine,
Turkey here is some evidence from animal and human studies that epidu-ral nonsteroidal anti-inflammatory drugs (NSAIDS) can produce analgesia without definite systemic side effects and neurotoxicity.
Method: After informed consent the analgesic effect ofepidural dipyrone (ED) 500 mg was investigated in intractable cancer pain, not responded to treatment with epidural morphine (12 mg) + bu-pivacaine (60 mg) and oral tramadol 150 mg/day. In addition, the analgesic effect of ED (500mg) given 24 hour after epidural lido-caine (100 mg) was investigated in Buerger patients. Ankle bra-chial indexes (ABIs) were also recorded before and after treatment using doppler flowmetry. Pam was assessed with VAS and percent pain score (control pain was accepted as 100%) at 0 (before treatment) and 15, 30, 45 min. and 1, 2, 3, 4, 5, 6 h. after treatment. ABIs were recorded before and 15 min. after treatment. Results: ED produced effective analgesia within 15 min. peaked at 30 min. and lasted 6 h. in cancer pain (ANOVA). In Buerger patients ED also produced effective analgesia than lidocaine. The patients in both groups were satisfied with the analgesia produced by ED. ED increased ABIs in both legs, but especially in leg with less vascular occlusion. In contrast, lidocaine decreased ABIs in both legs especially in leg with severe occlusion (ANOVA). Although systemic side effects and neurotoxicity were not observed, all patients suffered from transient pain at the catheter site and pin and needles in the legs. ED may be an alternative method in patients with intractable cancer pain and also in Buerger patients.
1. Anesthesiology 1993- 79:270-81.2. Anesth Analg 1998, 86, 117-8
DELIRIUM INCREASES THE EXPRESSION OF PAIN AND OTHER SYMPTOMS IN ADVANCED CANCER PATIENTS.
B. Gagnon*. P. G. Lawlor, I. Mancini*, J. Pereira*, J. Hanson*, E. Bruera, (SPON: A. Gamsa) Palliative Care Unit, Grey Nuns Community Hospital & Health Centre, Univ of Alberta, Edmonton, T6L 5X8, Canada.
Aim of Investigation: To investigate the expression of pain and other symptoms by patients with and without delirium.
Methods: 104 consecutive patients were prospecti-vely assessed for the presence of delirium upon admission and during their stay in the palliative care unit. Serial Mini-mental Status testing, standardized semi-structured interviews and DSM-IV criteria were used in evaluation of delirium. Symp-toms were assessed using the Edmonton Symptom Assessment Scale (ESAS) twice daily. The ESAS contains Visual Analogue Scale (0-100) scores for 9 symptoms (pain, activity level, nausea, depressed mood, anxious mood, drowsiness, appetite, wellbeing, shortness of breath). The ESAS scores during the episodes of delirium were compared to the scores of days without delirium.
Results: A total of 94 episodes of delirium with a median duration of 5 (3-10 : lower-upper quartiles) days occurred in 71 patients, while 33 patients remained delirium free, In 1520 out of 2376 patient-days, patients were able (alone or with help) to fill the ESAS at least once during the day. Mean ESAS pain scores during delirium and without delirium were 52 ± 24 vs 40 ± 21 respecti-vely (p= 0.0001). Mean ESAS scores for the other 8 symptoms were higher during delirium (p<0.001).
Conclusions: Patients who suffered from delirium express a greater level of pain and of other symp-toms than non-delirious patients, possibly due to disinhinibition. Not recognizing delirium in these patients may result in anappropriate administration ofopioids with the risk worsening delirium.
PAIN EVALUATION AND QUALITY OF LIFE IN PATIENTS SUFFERING FROM MESOTHELIOMA.
E. Pichard Leandri, C. Giraud*, G. Torloting', P. Poulain, P. Ruf-fie*, Institut Gustave-Roussy, 94805 Villejuifcedex, France. 'CHG - Hopital du Pare 57206 - Sarreguemines.
Introduction: This incidence ofmesothelioma has been on the increase during the last decade. Whatever the treatment, the outcome is fatal in a few months. During the course of the disease, moderate pains occur which gradually worsen until death.
Purpose: The objective was to study the incidence of pain and correlations between pain and the general condition, anxiety - depression and the quality of life in patients (pts) with a mesothelioma so that palliative treatment would be improved.
Patients and Methods: A prospective study was conducted over 15 months and data were collected using a computerized file “ AlgoAK ”. The patient's general condition (Kamofsky index), pain: characteristics and evaluation [VAS Mac Gill, body outline), anxiety-depression (Hamilton scale), the quality of life (EORTC) and treatment. Pain characteristics were analysed and possible correlations were sought between these different variables.
Results: Twenty-two pts (13 male, 9 female) were entered on the study. Seven-seven percent were experiencing pain and men previously exposed to asbestos had more intense pains. Pain had no impact on the quality of life, nor on anxiety-depression. The three scales: clinical status, general status and quality of life were correlated and mutually influenced each other, independently of pain.
Discussion: As the number of items chosen were multiple, to date, the cohort is not sufficiently large to allow conclusions to be drawn. The AlgoAK file is probably too exhaustive for this analysis.
Conclusion: Malignant mesothelioma is a painful disease and men previously exposed to asbestos experience the most severe pain. Thoracoscopy, the current diagnostic tool, generates more excruciating neuropathic pain. Changes in the quality of life during the course of the disease are independent of pain.
Acknowledgments: Work supported by a CRC IGR n° 9616 funding and ARC research grant n° 1108
A SUPERPOTENT TOPICAL STEROID FOR CONSTRICTING BREAST CANCER SYMPTOMS
Gilbert R.Gonzales*, Andrea Cheville*. (SPON: Kathleen Foley), Memorial Sloan-Kettering Cancer Center, 1275 York Ave, New York, New York, USA
Aim of Investigation: We have recently used the topical superpo-tent corticosteroid clobetasol (Temovate®) for treating constricting pressure symptoms and pain associated with breast carcinoma in two patients. Both patients responded with dramatically reduced pressure sensation and swelling with pain resolution.
Methods: Our first patient was a 56 year-old woman with inflammatory breast carcinoma with skin invasion and spread circumfer-entially around the neck. She experienced a profoundly distressing sense of throat constriction, pressure and strangulation with associated air hunger. Opioid analgesics, anti-anxiety agents, and paren-teral steroids failed to resolve the progressive symptoms described. A palliative tracheostomy was considered due to the patient's extreme distress. However, a trial of topical clobetasol applied topi-cally twice daily was initiated prior to this procedure. As per the manufacturer's recommendation, in order to avoid dermal atrophy, clobetasol therapy was applied for 2 consecutive weeks followed by a 5-day hiatus before resuming therapy. The second patent is a 52 year-old woman with intraductal breast carcinoma and right mastectomy. Local recurrence to the right chest wall and axilla produced a nodular mass with resulting pain, constriction, and diminished arm range of motion. High-dose opioid rotation and non-steroidal anti-nflammatories failed to ameliorate her symptoms. A trial of twice daily topical clobetasol to the affected area was initiated.
Results: At 3 days after the initiation of clobetasol, our first patent experienced a 5-point decrease in her visual analogue (VAS) pain rating to 3 over 10, increased cervical range of motion, diminished air hunger, and a reduction in base of neck circumference. The patient continued to respond to clobetasol with complete resolution of her symptomatology until her death 4 weeks later. In the case of the second patient Clobetasol therapy reduced the patient's VAS from 8 to 2 out of 10. She experienced a marked escalation of her pain during the requisite 5-day clobetasol withdrawal, which resolved with reinitiation of therapy.
Conclusion: Clobetasol or other superpotent topical steroids may have a role in the terminally ill patient with constricting breast cancer symptoms. In our two patients, both had good pain relief with the added benefit in one patient of reduced neck pressure, reduced sensation of strangulation and air hunger and measurable reduction in her neck swelling.
CHARACTERISTICS OF PATIENTS REFERRED TO A PALLIATIVE CARE UNIT IN DENMARK
M Groenvold, AK Olsen. L Pedersen, S Rydahl, P Sjogren (SPON: AB Thomsen), Dept. Palliative Med., Bispebjerg Hospital, Copenhagen, Denmark.
Aim of Investigation: To characterise the cancer patient's symptoms when referred to a Danish palliative care unit.
Methods: In 1998 we started a longitudinal study of all patients referred for in-patient care in our palliative Dept. We report the characteristics of 56 patients, all having advanced cancer. Their median Kamofsky Performance Status was 40. When admitted to the unit, patients were asked to define the five symptoms and psy-chosocial problems they considered most important for their current situation. Patients were given self-assessment questionnaires. Edmonton Symptom Assessment System (ESAS) which consists of nine 0-100 visual analogue scales, range 0-100 mm; 100 mm represents maximal symptomatology. The EORTC QLQ-C30, a health related quality of life questionnaire, is also scored from 0-100. 100 representing good functioning).
Results: The numbers of patients selecting each symptom/problem were: Pain: 50 patients (pts.). Fatigue: 39 pts. Lack of appetite: 19 pts. Nausea: 17 pts. Reduced physical functioning: 16 pts. Dysp-nea: 16 pts. Inactivity: 10 pts. Depression: 8 pts. Drowsiness: 7 pts. Vomiting: 7 pts. Dry mouth: 7 pts. Constipation: 7 pts. Other symptoms were selected less frequently. Of the 56 pts., 49 filled in the ESAS when admitted and had the following mean scores: pain 56, inactivity 78, nausea 31, depression 36, anxiety 38, drowsiness 61, lack of appetite 69, lack of well-being 67, shortness of breath 45. The EORTC QLQ-C30 was filled in by 41 patients. The function are given in mean scores. Physical Function 30, Role Function 14, Emotional Function 53, Cognitive Function 41, Social Function 39, Global Health Status/Quality of Life 35. Selected EORTC symptom mean scores: Fatigue 80, Sleeping difficulties 41, Constipation 41, Diarrhoea 24.
Conclusion: As seen on the 2 physical symptom assessment scores the patients had a multidimensional and severe symptomatology, and this severely reduced their quality of life as measured by EORTC QLQ-C30.
INTENSITY AND ETIOLOGY OF SYMPTOMS DURING CANCER PAIN TREATMENT FOLLOWING WHO-GUIDELINES.
Stefan Grond. Thomas Meuser, Petra Stute*, Nathalie Schmidt*, Rainer Sabatowski, Lukas Radbruch, Klinik fur Anaesthesiologie, Universitat zu Koein, 50924 Koein, Germany
Aim of Investigation: Cancer pain treatment is often complicated by multiple other distressing symptoms. This study investigates prevalence, intensity and etiology of typical symptoms.
Methods: 593 cancer patients being referred to an Univ based pain clinic were included. Pain therapy followed WHO-guidelines; other symptoms were treated systematically by antiemetics, laxatives, neuroleptics and other drugs. Symptom intensity was measured daily by self-assessment. Symptom etio-logy was assessed weekly by the pain clinic.
Results: The patients were treated for 30,335 days using WHO-step 1 at 8%, step 2 at 29%, step 3 at 55% and only adjuvants at 8% of days. Efficacy of pain treatment was good in 70%, satisfactory in 16% and inadequate in 14% of patients. The prevalence of all symptoms was reduced during treatment in comparison to the assessment at admission.
| Symptoms: | Etiology | Intensity | ||||
| A | A&C | C | 1 | 2 | 3 | |
| Anorexia | 11% | 2% | 0% | 4% | 5% | 4% |
| Constipation | 4% | 6% | 14% | 9% | 10% | 5% |
| Nausea | 8% | 8% | 5% | 11% | 7% | 3% |
| ZNS | 10% | 15% | 5% | 10% | 12% | 8% |
| Pruritus | 3% | 2% | 1% | 2% | 3% | 1% |
| Urinary | 6% | 0% | 0% | 2% | 2% | 2% |
| Vomiting | 4% | 4% | 2% | 4% | 4% | 2% |
| Sweating | 12% | 3% | 2% | 7% | 6% | 4% |
Percentage ofn = 30,335 days. A: induced by analgesics, C: caused by cancer, 1 mild, 2 moderate, 3 severe, ZNS: confusion, drowsi-ness, dizziness.
Conclusions: Prevalence and intensity of symptoms can be reduced by cancer pain treatment in combination with systematic symptom control. These symptoms are caused most often by pain treatment or cancer disease.
NURSING SUPPORT STRUCTURE FOR OPTIMAL INTRATHECAL PAIN TREATMENT.
M. Judong. K. Vissers, C. De Deyne*, M. Puylaert, J. Van Canneyt*, J. Froyen*, R. Heylen*, Pain Service, Dept of Anaesthetics, ZOL, Schiepse Bos 6 3600 Genk, Belgium
Introduction: If a good support structure is offered by nurses and anesthetists, terminal cancer patients may return and stay at home after the insertion of an intrathecal subcutaneous tunneled catheter with an external PCA pump for long-term home based terminal care. In all patients the WHO-guidelines were applied and failed.
Aim of Investigation: (1) To evaluate a home-based invasive pain treatment technique, (2) the necessary support structure, and (3) to examine the evolution of the pain (VAS) and the functional parameters of life (Kamofsky Performance Status score, KPS).
Method: Since 1996 all contacts with these patients were systematically registrated by the Pain Nurse of the hospital. So it was possible to include 50 patients in our retrospective (January 96-July 98) and descriptive analysis.
Results: Twenty-four patients (48 % of our study group) returned home after catheter insertion and survived a mean period of 90 days. We could not find a relevant correlation between the VAS and the KPS. Nevertheless we observed that continuous intrathecal administration ofbupivacaine: morphine (3:1 mg/ml) not only controled the pain, but also stabilized the functional parameters of life, despite the progression of the disease. We observed an immediate decrease of the VAS from 7.62 to 2.94 and this remained significantly lower until one week before death. The KPS remained stable (m 45%, SD 5) until three weeks before death. Once a significant decrease of the KPS and an important increase of the VAS (not caused by a catheter related problem) occured, death of the patient was mostly not far away. In this terminal phase of life, the total daily dose ofopioids and local anesthetics had to be adjusted to a higher dose and additional therapies had to be instituted without delay.
Conclusion: In intrathecal administration of analgesics (opi-oids/local anesthetics) for terminal cancer patients a well established support team of nurses and anesthetists is essential to provide an adequate end of life pain treatment, as well as to prevent catheter related problems.
Acknowledgment: Awarded with the 'Asta Medica Price 1998, Nursing and Chronic Pain'.
CONTINUOUS SUBCUTANEOUS OPIOID INFUSION (CSOI) FOR 1320 CONSECUTIVE PATIENTS.
P.A. Keefe and C.G. Merridew. Depts of Pharmacy and Anaesthesia, Launceston General Hospital (LGH) Launceston, Tasmania 7250 Australia.
Aims: For all palliative care CSOI in the region's 130,000 population, April 1987- March 1998, to: 1) Document patient, location, diagnosis, CSOI duration, and the drug(s) infused; and 2) Estimate CSOI efficacy, safety, practicability and cost.
Introduction: Polypropylene syringes ofopioid (plus any added drugs), for > 97% of patients were filled by Pharmacy in batches of up to 6 days' supply. In hospital or at home, CSOI was by Graseby MS16A syringe driver loaned from a regional pool, now of 47.
Study Methods: Pharmacy data identified nearly all CSOI cases, and telephone queries the remainder. Tasmania's Cancer Registry gave regional cancer-deaths (total, and by primary tumour) and LGH data the CSOI-cancer diagnoses. Problem detection was by report to the Pharmacy. 569 unused syringes were sterility-tested.
Results: Morphine (1303) or fentanyl (17) were used for the 1320 CSOI cases (now ” 150/year), costing US$11 per daily syringe. There were 197 non-cancer cases. For all cases, mean duration was 18 days (median, 6). Compatibility-tested CSOI mixtures were:morphine + SI ofdroperidol, dexamethasone, Buscopan or mida-zolam (see Targett et al}. All sterility-tests were negative. Known morbidity was extrapyramidal reactions in 9/1057 droperidol patients. Regardless of primary tumour, from 1991 half the region's cancer patients/year had CSOI. In 1987, 88% of CSOI began in the LGH; but since 1995, 60% of CSOI each year was started by family doctors outside the LGH and supervised by community nurses.
Conclusions: CSOI was common in cancer, but rare for other dying patients. CSOI seemed effective, versatile, inexpensive, and remarkably trouble-free .
References: Targett PL, Keefe PA, Merridew CG. Compatibility and stability of drug adjuvants and morphine tartrate in 10 ml polypropylene syringes. Australian Journal of Hospital Pharmacy 1997, Vol. 27 No.3: p. 207-212.
APPLYING THE AMERICAN PAIN SOCIETY'S QA STANDARDS TO EVALUATE THE QUALITY OF PAIN MANAGEMENT AMONG SURGICAL, ONCOLGY, AND HOSPICE INPATIENTS IN TAIWAN
Chia-Chin Lin. School of Nursing, Taipei Medical College, Taipei, Taiwan.
Aim of Investigation: To apply the American Pain Society (APS) outcome questionnaire to examine and compare the quality of pain management provided in surgical, oncology, and hospice inpatient units in Taiwan.
Methods: The APS outcome questionnaire was used to evaluate the quality of pain management among 100 surgical, 100 oncology, and 34 hospice inpatients in Taiwan.
Results: Significant differences in pain severity ratings (worst pain, least pain, pain now, and difference between worst pain and least pain) as well as patient satisfaction with pain management was found among these three groups of patients. Correlations between pain levels and satisfaction were small or insignificant. The distribution of patient satisfaction scores was highly positively skewed.
Conclusions: No matter in which country the APS outcome questionnaire is being used, it may need to be combined with other measures.
Acknowledgments: Supported by Grant 86-2314-B-03 8-030 from the National Science Center of Taiwan.
EFFECTS OF ORAL NALOXONE ON OPIOID-INDUCED CONSTIPATION AND SMALL BOWEL TRANSIT TIME.
Maywin Liu. Eric T Wittbrodt, Depts of Anesthesia, St. Joseph Hospital, Baltimore, MD 21204, Univ of Pennsylvania, Phila, PA, Philadelphia College of Pharmacy & Science, Phila, PA 19104, USA
Aim of Investigation: To evaluate the effect of oral naloxone on opioid-induced constipation and small bowel transit time.
Methods: In a double-blinded, randomized, placebo-controlled study, cancer and non-malignant pain patients on stable doses of opioids with complaints of constipation were assigned to one of the following groups: 1)4 mg TID oral naloxone, 2) 2mg TID oral naloxone, or 3) TID placebo. Baseline pain scores, opioid use,and bowel habits were assessed prior to beginning the study and then daily. Small bowel transit time was measured using the lactulose hydrogen-breath test (LHBT) prior to the study and repeated the last day of the study.
Results:
| Pt# | Drug | Baseline BM/wk | Study BM/wk | Pain | chang inLHB |
| 1 | Placebo | 3 | 5 | Increased | None |
| 2 | 4 mg naloxone | 5 | 7 | No change | None |
| 3 | 4 mg naloxone | <1 | 1-3' | Increased | N/A" |
| 4 | Placebo | 2 | 0^ | Increased | N/A"1 |
| 5 | 4 mg naloxone | 4 | 6 | No change | None |
| 6 | 2 mg naloxone | 1 | 3 | Increased | None |
| 7 | Placebo | 1 | 1 | No change | None |
| 8 | 2 mg naloxone | 2 | 5.5 | No change | None |
*stopped after 2 days due to analgesia reversal and diarrhea;^stopped after 3 days due to reversal of analgesia, ** post-LHBT not obtained due to early discontinuation of study drug
Conclusion: Oral naloxone appears to be effective in reversing opioid-induced constipation. Its main effect appears to be in the colon.
Acknowledgment: Supported in part by a grant from the American Cancer Society.
HOME PALLIATIVE CARE AND MORPHINE INFUSION: NETWORK MANAGEMENT
Veronique Mailland*. Nadine Memran, Marie-Josee Daniel-Rosset, Helene Femandez*, Pain Dept, CHU Nice, 06000 Nice, France
Background: Infusion of morphine by pump in the home care is often a difficult problem. In this retrospective study, the outcome of morphine therapy has been analysed in 28 patients.
Methods: During 12 months, 28 patients were included in the study. Management of home care consisted of an organization of a network with health professionals by supporting and coordinating the already existing healthcare structures with multidisciplinary team approach.
Results: Network was established after the first visit in pain management Dept. Quality evaluation of management home care is periodically undertaken by all practitioners and health professionals involved in our programme. For each patient, amounts of morphine, pain and symptoms assessment were recorded in a "livert:pompe a morphine". Questionnaires were administered every week.
Conclusion: Home palliative care and morphine infusion require a specially trained and solid interdisciplinary team. Network allows terminally ill patients to stay at home.
SYNERGISM AND ANTAGONISM OF COMBINED THERAPY OF MORPHINE WITH DEANXIT DURING MEDICAL TREATMENT OF CHRONIC PAIN IN ON-COLOGIC PATIENTS
N. Manolov, N. Hristov, Urgent Medical Dept of 28th Polyclinics, Sofia 1582, Bulgaria
Aim of Investigation: Relieving pain is a major part of the treatment ofoncologic patients. The investigation focuses on the following: 1) whether the combined treatment ofDeanxit with Morphine affects the degree of analgesia as compared with the Morphine monotherapy; 2) the impact of the combined therapy on the depression syndrome; 3) the interaction between the Deanxit cholinolitic effect and the Morphine vagus effect. Methods: A contrastive method was applied to check validity of hypothesis in a standardised observation of groups of patients. The first one, on Deanxit and Morphine medication, consisted of 277 patients, while the second one, only on Morphine medication, consisted of 192 patients.
Results: In the first group, the acuteness of pain decreased with 184 patients, which allowed for a reduction of the Morphine dosage and brought about a delayed development of tolerance. In the second group, the acuteness of the pain decreased by the same degree with 126 patients. The frequency of occurrence of the depression syndrome in the first group was 21%, while it was 38% in the second group. The occurrence ofbradicardia and bradipnoea was 17% and 23% respectively for the first and the second groups.
Conclusion: 1) The combination ofDeanxit with Morphine is efficacious in mild and medium cases; it improves the rate of pain relief by 19% more than the Morphine monotherapy. This combination has a blocking effect on the emotional reaction to pain and a positive influence on the mood of the patient. 2) The combined therapy reduces the occurrence of the depression syndrome and can also prevent its appearance. 3) The two medicines exhibit syner-gism in respect to their analgesic effects, and the mild and moderate m-cholinolitic effect of Deanxit help to neutralise the central vagus effects of Morphine.
CONTINUOUS SUBCUTANEOUS OPIOID INFUSION (CSOI): A 76-CASE PROSPECTIVE AUDIT.
C.G. Merridew. P.A. Keefe, J. Allford*. Anaesthesia, Pharmacy, & Community Nursing: Launceston General Hospital (LGH) Tasmania 7250 Australia.
Aim: To prospectively record why, where & how palliative care CSOI was conducted (in a community of 130,000), its efficacy and problems, and to estimate its cost-effectiveness.
Methods: CSOI had evolved in the region since 1986, by integrating LGH Pharmacy with regional medical & registered nurse (R.N.) care. Half the region's cancer palliative care patients have CSOI. The study was institutionally approved. Data was obtained from: (i) Pharmacy's list of all regional CSOI cases (li) telephoning the initiating doctor, and (iii) at intervals, 'phoning the person who supervised the case day-to-day. For outpatients on CSOI, material & R.N. costs and inpatient days saved were estimated.
Results: There were 76 consecutive fully-audited patients. For 60 preceding pilot ones, only the "Initiating" data was complete; it agreed with the audit's. For the 76+60 cases, 47 family doctors started 80/136 CSOI. Previous slow-release oral morphine: 85. For the 76 audited cases, the initial opioid was morphine in 92%. Main CSOI indications were: inadequate symptom relief, 46%; can't swallow but lucid, 26%; to establish oral morphine dose, 12%. There were 308 outpatient CSOI-days and 468 inpatient days. Of the 76 cases, only 4 were problematic; 3 had unacceptable side-effects, fixed by changing back to oral, and 1 had poor SCOI absorption, fixed by using an existing I.V. portal. Costs/savings were:(i) R.N. visits/week for CSOI, 7 (range 3-14) (ii) Syringes, dressings & pump for the 10 CSOI days/case (iii) > 250 inpatient days saved.
Conclusions: Now usually started by family doctors, CSOI therapy was orthodox, effective and low-cost. Acknowledgments: Funded in part by the Clifford Craig Medical Research Trust, Launceston Tasmania.
CANCER PAIN MANAGEMENT IN COLOMBIA: A NATIONWIDE SURVEY
Jairo Moyano', Franklin Ruiz2, Anneli Vainio3, 'National Cancer Inst, Bogota, Colombia, rational Univ of Colombia, ^ept of Anesthesia, McGill Univ, Montreal, Quebec, Canada
Introduction: A questionnaire containing 7 open and 19 multiple choice questions was sent to a random sample of 3000 Colombian physicians treating cancer patients. Questions include characteristics about cancer pain administration ofopioids, dependence problems and source of education in the treatment of cancer pain. The knowledge of the methods of cancer pain therapy were evaluated as well as the ability to apply their knowledge by studying their suggesting treatment of 3 simulated patient cases.
Results: The favorite drugs were "weak" opioids (2nd step) for bone pain and for severe pain caused by melanoma. The preferred treatment for neuropathic pain caused by rectal carcinoma was nerve blocks with local anesthetics. 46% identified lack ofopioids in the pharmacy; dependence problems were seen in 36% and 4% of the doctors say they never prescribe opioids the booklet cancer pain publisher by the how was a unknown for a 47% of the physician; 67% of the doctors regarded their education in cancer pain as insufficient
Discussion: The aim of the study was to examine how cancer pain is treated in Colombia where there are difficult conditions for opioid prescription and availability and polarized attitudes towards opioids in the sociality because of illegal drugs problems. The sample was representative but the response rate was low and can be interpreted as an indicator of the lack of interest of the physicians and the fact that only very few doctors gave detailed suggestions to the patient examples show lack of knowledge and or confidence to answer a questionnaire; opioid addiction was seen as a problem by many physicians and this fear can be of crucial importance in medical education; since cultural and legal connotations of the expressions narcotic and drug are particular in Colombia and Latin America countries, this situation is an additional barrier to cancer pain treatment.
Conclusions: The majority of Colombian physicians seem not to be interested in research in cancer pain; pharmacological treatment is the mainstay but choosing doses seems to be a major problem; opioid availability is not sufficient; concerns about addictions are highly prevalent. The knowledge of Colombian physicians in pain relief is insufficient and newer methods to educated and motivated physicians are waiting for further developments.
PAIN ASSOCIATED WITH CARCINOMA-INDUCED MENINGITIS LINKED TO SOLID CHILDHOOD TUMOURS. DIAGNOSTIC MODALITIES.
E. Pichard-Leandri. (Spon: C. Wood) V. Schmitz1*, C. Schoep-fer*, J. Grill*, A. Gauvain Piquard, Institut Gustave Roussy, 94805 Villejuifcedex, France. 'Hopital de la Citadelle, Liege, Belgique.
Introduction: Carcinoma-induced meningitis is particularly frequent in children presenting neurological tumours at the terminal stage. Early and the least invasive of diagnostic procedures allows appropriate pain management.
Purpose: The aim of this study was to ascertain whether diagnostic procedures perfected in adult patients (pts) in 1996 were equally effective in children.
Methods: All children suffering from diffuse pain were referred to the pain management consultation and followed up until death. Pain was evaluated using a visual analogue scale (VAS) for children older than 5 years and the DEGR01 for children younger than 5. A body outline drawing was used to pinpoint pain whenever possible. The examination already used routinely was adapted according the age of the patient and degree of cognitive impairment.
Results: Currently, 20 children have been included in the study but the results concern the first 10. All pts had a neurological tumour and all of them presented a mixture of pains. Nociceptive pain was discovered at palpation of the vertebral column (D4 D5). Other pains were affecting the shoulders, arms and the popliteal spaces. Mosaic neuropathic pain was found in all cases. Obvious mosaic allodynia was found on the drawings of 7 children. Severe sub-occiptal allodynia was found in 3 pts with associated sympathetic symptoms. The diagnosis was confirmed in 3 cases on the lumbar puncture. In 5 cases, the clinical examination and imaging studies sufficed and in 2 cases, the diagnosis was based exclusively on the clinical examination.
Conclusion: Early diagnosis of carcinoma-induced meningitis does not modify life-expectancy but allows better control of pain and the child's quality of life is improved. (1) Douleur Enfant Gustave Roussy®
TRANSDERMAL FENTANYL IN HOSPICE: A SURVEY OF RESCUE DOSING AND PAIN CONTROL
Marti Robards. Visiting Nurse Association Hospice Care, St. Louis, MO, USA, SPON: Jack F. Schreckengost, Purdue Pharma L.P, Norwalk, CT, USA
Aim of Investigation: To evaluate rescue medication use and pain control in hospice patients treated with the transdermal fentanyl patch.
Methods: Case records for hospice patients receiving fentanyl transdermal system (TDSF, Duragesic®) as the primary analgesic were reviewed in March 1996, October 1996, and September 1997. TDSF was titrated as per labeling guidelines. Patients were queried about medication use and pain control during hospice nurse visits. Results: Records from 25 patients (aged 48-97 yr.) were surveyed. Most patients (76%) experienced cancer pain and 88% could tolerate oral medications. Patients received TDSF for approximately 30 days. Doses of TDSF were titrated from 87 ug/hr (enrollment) to 111 ug/hr (final) (range, 25-400 ug/hr).
| Table 1: Rescue use and | pain control. |
|
| Mean (SE) | Range | |
| Daily rescue doses | 7.0 (0.7) | 1,20 |
| Current pain | 1.1(0.2) | 0,5 |
| Pain at rest | 1.6(0.3) | 0,4 |
| Pain during activity | 2.0(0.3) | 0,5 |
| Pain score: 0=no pain, 1=mild, 2=discomfort, 3=distressting, 4=homble, 5=excruciating | ||
Morphine oral solution was the most common rescue analgesic. Doses ranged from 5-140 mg, increasing as disease progressed. 8 patients required rescue every 1 to 2 hrs; on 26 assessment days. 11 patients reported uncontrolled pain (score 4 or 5) on at least 1 day.
Conclusions: While pain control was good in these hospice patients, the use of rescue medication was relatively high despite increasing doses ofTDSF.
TREATMENT OUTCOME OF PAIN AND OTHER SYMPTOMS IN ADVANCED CANCER PATIENTS.
P Sjogren. AK Olsen, M Groenvold, L Hermann, L Pedersen. (SPON: ME Crawford) Dept. Palliative Med. Bispebjerg Hospital, Copenhagen, Denmark.
Aim of Investigation: To evaluate the treatment outcome concerning pain and other symptoms in cancer patients in our dept. Palliative Medicine.
Methods: Pain is one of the most frequent and serious symptoms in patients with advanced cancer. Approximately 75% of cancer patients admitted to our Dept of palliative medicine accepted to take part in a longitudinal survey. When admitted for in-patient care, patients were asked which symptoms and psychosocial problems were most important. Of 49 patients filling in the first questionnaire (day 0), 40 patients stated that pain was one of the 3 most important symptoms. Of these 40 patients, 25 (63%) also filled in the Edmonton Symptom Assessment System (ESAS) (Bruera, 1991) one week later (day 7). ESAS consists of nine visual analogue scales. On each scale, values range 0-100 mm; 100 mm represents maximal symptomatology. Reasons for not filling in ESAS at day 7 were mainly that the patient had become too ill or had died.
Results: Of the 25 patients having complete data, 15 (60%) patients were judged to have neuropathic pain at day 0. At day 0, the mean ESAS pain score of the 25 patients was 56 mm. Mean scores on the other ESAS scales also revealed significant symptomatology: inactivity 78, nausea 29, depression 28, anxiety 36, drowsiness 55, lack of appetite 66, poor sensation ofwellbeing 69, shortness of breath 46 mm. At day 7, numeric improvements were seen in all ESAS scales. The mean score for pain decreased 14 mm (p=.02). The most pronounced improvements in mean scores on the other scales were for wellbeing, 20 mm (p=.004), nausea, 11 mm (p=.07), and anxiety 10 mm (p=.12). Interestingly, the improvement in pain was more pronounced in the 15 patients with neuropathic pain, 20 mm (p=.02), than in 10 patients not having neuropathic pain, 6 mm (P-.57).
Conclusion: After 1 week treatment in dept. of palliative care the cancer patients improved in all scales of ESAS. These preliminary findings based on a limited number of cases should be interpreted with care. Updated analyses will be presented.
14-DAY STABILITY OF MORPHINE TARTRATE PLUS NOVEL ADJUVANTS, MIXED FOR SUBCUTANEOUS OPIOID INFUSION (CSOI).
P.L.Targett* P.A. Keefe, C.G. Memdew (SPON: A.L. Doughty). Depts. of Clinical Chemistry, Pharmacy and Anaesthesia.Launceston General Hospital, Launceston, Tasmania 7250 Australia.
Aim: To test the stability of mixtures of morphine and novel adjuvants, used in palliative care CSOI, (Stability is known for morphine + dexamethasone, droperidol, midazolam and Buscopan formulations).
Methods: To morphine 400 mg, dexamethasone 4 mg, droperidol 2 mg, was added clonidine 450 mcg or ketamine 200 mg or ketoro-lac 30mg, plus 0.9% NaCI to 10 ml. Additional formulations, with morphine 40mg, were otherwise the same. All solutions were drawn up into 10 ml polypropylene syringes and stored in the dark at 21-23°C, or 4-8°C. A stability-indicating high pressure liquid chromatography (HPLC) assay using a photo diode array detector was developed, to measure the drug concentrations. Along with osmolality, pH and physical appearance, data points were obtained on Day 0, then about each 2 days for 14 days. Each data point was the mean of 6 assays. Stability of a given drug was defined as the loss of<10% of it's original concentration. Results: The mixtures of morphine plus all adjuvants (except ke-torolac) were stable for at least 14 days. The ketorolac mixtures at Day 12 contained a barely-visible colloidal precipitate, obvious by Day 14. There was no notable pH change. At 4-8°C, the ketorolac concentrations were >90% of original on Day 10 and 49% on Day 14. A light yellow coloration developed in the 400mg morphine/10 ml solutions stored at 21-23°C, but dmg content was unaffected.
Conclusion: All drugs in all mixtures were stable for at least 10 days, stored in the dark at 21-23°C, or 4 -8°C. Acknowledgment: Supported in part by the Clifford Craig Medical Research Trust, Launceston, Tasmania.
Reference: Targett PL, Keefe PA, Memdew CG. Compatibility and stability of drug adjuvants and morphine tartrate in 10 ml polypropylene syringes. Australian Journal of Hospital Pharmacy 1997, Vol. 27 No.3: p. 207-212.
PREVALENCE OF PAIN IN PATIENTS WITH ACTIVE CANCER IN SCOTLAND: A NATIONAL CROSS SECTIONAL SURVEY
John Welsh. Marie Fallen, Paul Stroner, David Brewster, Anne Gould, Stephen Hutchison, Michael Combleet, Barbara Dymoch, Elizabeth Porterfield, Mhoira Leng. National Pain Audit Working Party, Scotland, UK.
Aim of Investigation: To conduct a population survey in patients with active cancer and establish prevalence and severity of pain across 6 different settings; degree of compliance by prescribers with guidelines for pain control adapted from the World Health Organisation's recommendations; relationship between compliance with these guidelines and level of pain control.
Methods: After local and multicentre ethical approval patients were recruited from six different settings. Scotland was divided into five regions and numbers of patients required in each setting in the five regions was calculated to give adequate statistical power to detect differences of at least 10% among those with controlled pain. A random sample of hospitals was selected for participation. General Practitioners were selected at random and approached to identifying a sampling frame for the community settings. Research assistants recruited patients and collected data according to a proforma with agreed definitions. Patients assessed their own pain using the Wisconsin Brief Pain Inventory. Prescribing records were checked with 15 prescribing standards and violations noted.
Results: 47% of general practitioners responded to an explanatory letter and of all GPs contacted only 20% supplied patients. 20% of patients declined to participate. 953 patients were recruited, 196 from the community, 250 from oncology centres, 231 from acute hospitals and 276 from specialist palliative care units. Detailed analysis of the data from these 953 patients is ongoing and will be presented.
Conclusions: This is one of the largest prospective audits ever conducted, crossing different clinical settings where'cancer pain is managed. The timeliness of the initial gathering of data has allowed a base line to be identified. The Scottish Intercollegiate Guideline Network is to publish guidelines for the management of pain in patients with cancer. A repeat of the audit will allow an assessment at a clinical level of the impact of these guidelines.
Acknowledgments: Funded by a grant from the Clinical Resource & Audit Group (CRAG), The Scottish Office, Dept of Health, Edinburgh EH1 3DG. The views are those of the authors and not the funding body.
NEW INITIATIVES IN THE IMPROVEMENT OF CANCER PAIN RELIEF AND PALLIATIVE CARE IN EASTERN EUROPE
Jacek Luczak*, Aleksandra Lemieszek-Kotlinska, Ewa Baczyk*, Maciej Kluziak*, Palliative Care Dept, Univ of Medical Sciences, Poznan, 61-878 Poznan, Lakowa 1/2
Aim of Investigation: To investigate the impact of regional courses in palliative medicine and of the Poznan
Declaration on the adoption of World Health Organisation (WHO) guidelines on cancer pain control and palliative care in eastern Europe.
Methods: Since 1990, the Palliative Care Dept of Poznan and the WHO centre Sir Michael Sobell House, Oxford, have collabora-tively organised an annual course in palliative medicine in the English language for professionals from eastern Europe, where the skills of caring for the dying are still undeveloped. The annual course is an opportunity to present achievements and to discuss obstacles to the improvement of cancer pain control and palliative care. The Poznan Declaration is an important document which was drafted by representatives of Belarus, Bulgaria, the Czech Repub-lik, Hungary, Latvia, Lithuania, Poland, Slovakia and Romania in a special workshop chaired by Dr lan Stjemsward at the 1998 course in Poznan. The Declaration comprised a report from each country in respect of national policy, opioid availability, palliative care services, education in palliative care and public awareness. A Task Force Group was formed of the leaders in palliative care in each country represented, in order to initiate change. Questionnaires designed to cover the above-mentioned parameters and group meetings are methods by which progress - and also obstacles to progress - may be monitored.
Results: The Declaration has been translated into the languages of the participating countries; policies on cancer pain control and palliative care developed in Hungary and Poland were disseminated and used in negotiation with health service administrators. Each year, the data collected show an improvement in the availability of immediate-release and slow-release morphine and a parallel development in services and education. Progress in changing national policies in relation to palliative care remains slow.
Conclusion: The organisation of regional courses in palliative medicine, in conjunction with such documents as the Poznan Declaration and its associated Task Force, have greatly assisted the development of palliative care in eastern Europe.
INFLUENCING CANCER PAIN MANAGEMENT:MEDICAL WRITING IN THE SECOND HALF OF THE 20™ CENTURY
Christina Faull. St. Mary's Hospice, and Cancer Studies Univ Birmingham, Birmingham B29 PDA, UK
Aim of Investigation: To investigate qualitative and quantitative changes in medical writing about cancer pain since the 1950's in non-specialist journal publications and undergraduate textbooks.
Specific attention was given to the influence of the discovery of the endogenous opioids and their receptors.
Methods: Manual and electronic analysis of the contents of the Lancet, British Medical Journal and New England Journal of Medicine; Manual review and comparison of medical texts.
Results: Journal articles focusing on cancer pain have increased from 0.01% in 1966-70 to 0.09% in 1991-1995. The percentage relative to other articles on pain or cancer has increased more markedly. Absolute numbers of articles, particularly original research, remain low. Textbook material has altered considerably both in content and quantity. Teaching about pain has progressed from consideration solely as a clue to a diagnosis, to discussion of the phenomena of pain and of pain relief. This is, however, remarkably variable. The reluctance to use morphine for fear of addiction is long lived. Indexed entries and the text are dominated by addiction, intoxication and other negative images of morphine.
Conclusions: The discovery of the opioid receptors, leading to increased understanding of the mechanisms of action of morphine and other opioid analgesics is reflected generally in medical textbooks. These discoveries have had little influence on medical writing specifically about cancer pain.
Acknowledgments: Supported by Wellcome Trust Research Fellowship in History of Medicine.
9th WORLD CONGRESS ON PAIN, 1999, Vienna, Austria, p.562 - 569