|
EFFECT OF SURGEONS PRESCRIBING PATTERNS ON POSTOPERATIVE OPIOID ADMINISTRATION
Andrew Amata. Linda Samaroo, Sharon Monplaisir, Public Hospitals, Georgetown and New Amsterdam,
Guyana South America
Aim of Investigation Surgeons differ in their postoperative analgesic prescribing patterns
This may influence nurses' compliance with opioid administration
Method We studied patients who underwent surgery that was expected to cause pain of moderate
to severe intensity and require opioid analgesia. The medication chart on which the prescribed and administered
doses of medication are recorded were collected and analyzed
Results We studied 350 patients treated by 9 different surgeons Route of opioid administration
was intramuscular in all the patents The prescription patterns could be broadly classified into
two, a fixed amount of opioid to be administered at regular intervals and a fixed amount to be
administered as required (pm) In both groups the scheduled prescriptions were seldom followed,
with the administered daily doses usually less than the prescribed doses. Only 4% of patients
received the prescribed dose The difference between prescribed and administered opioids was greater
in the pm group than in the regular interval group (p<0 05). All the surgeons generally underprescnbed
opioids and in both groups many of the patients experienced significant pain
Conclusion The "ideal" pain prescription is yet to be devised. Regular interval prescnptions
tended to compel the nursing staff irrespective of workload, to interact with the patient concerning their
pain. PRN dosing is less efficient as it requires the conscious effort of either the patient or the nurse
or both to effect treatment
RATIONALISING INTRAVENOUS MORPHINE PRESCRIPTIONS IN CHILDREN
B J Anderson*, M.A. Persson*. M Anderson*, A L Garden* (SPON Waddell), Pain Service, Dept of Anaesthetics,
Starship Children's Hospital, Park Road, Auckland, New Zealand
Aim of Investigation A morphine dose-analgesic effect response curve for children has not been
descnbed The individual variability ofpharmacokmetic and pharmacodynamic parameters means each child requires
individual assessment and management Consequently, small incremental intravenous doses of morphine are
often titrated to a satisfactory analgesic endpomt In order to achieve such dosing flexibility we have
recently introduced an intravenous opioid policy to our hospital An audit of the protocol was performed
Methods A two month prospective chart review of all children prescribed morphine was undertaken
following the introduction of the intravenous opioid policy and these data were compared with
historical controls from a three month period prior to the protocol's introduction
Results Demographic data of children before and after implementation of the protocol showed
no difference between the two populations Mean daily morphine doses administered were similar
in both the pre-protocol and protocol time penods The administered dose distribution for the pre-protocol
and protocol prescriptions were similar. A greater proportion of children were given morphine
on the first postoperative day when the protocol was used No adverse effects in either group were
noted
Conclusions. Drug errors are a consequence of system error and goals of zero drug error
rates should be aggressively sought with systems in place that seek to eliminate the effects of
inevitable human error This opioid protocol is one such system Acknowledgments Starship Children's
Hospital
CHANGING FROM I.M. TO NURSE CONTROLLED I.V. MORPHINE ON WARD - IS IT DANGEROUS?
Petter C Borchgrevmk*. Bjam Hval*, Ase Jystad* and Pal Klepstad* (SPON N. Bemer), Pain Clinic, Dept
ofAnaesthesiology, Umv Hospital, Trondheim, Norway
Aims of the investigation To evaluate continuation ofi.v. morphine titration from 1CU
to the ward It was focused on pain control and respiratory depression since i v morphine has been
considered to be dangerous outside ICU This new regimen was necessary since i m opioids are known
to be insufficient and because all patients can not receive continuous epidural analgesia (CEA)
or PCA after major surgery
Method Before leaving 1CU, all patients still in need ofi v morphine got a monitoring
flow sheet for the ward This sheet also used for CEA and PCA, was designed to observe pain, respiratory
depression, sedation and BP every third hour before and after i v morphine titration The nurses
were allowed to give 2,5 mg morphine each 5 minute if patients had respiratory rate(RP) > 8/mm
without heavy sedation and presented more pain than 2 on VAS (0-10) This titration was continued
until the patients presented VAS less than 3 or R?<8 or heavy sedation
Results Dunng the first half-year of observation, 215 patients received morphine titration
the 9 first hours (6h-48h) on ward This presented 7% of all patients operated on Depts of Surgery
and Orthopedics, while 11% received ECA and 1% PCA None presented morphine-induced respiratory
depression or heavy sedation The patients received in average 11 mg morphine (2,5-62,5), and their
pain score were in average 4,5 before and 1,4 after titration
Discussion So far i v titration with morphine seems safe on ward and assures good pain control
However, this regimen is further evaluated for presentation of more data
OPTIMAL DOSE OF NALBUPHINE FOR TREATMENT OF PRURITUS INDUCED BY INTRATHECAL MORPHINE FOR
POSTOPERATIVE PAIN RELEIF
Somrat Charuluxananan. Oranuch Kyokong Dept of Anesthesiology, Faculty of Medicine, Chulalongkom Univ,
Bangkok 10330, Thailand
Objective. To determine the optimal dose ofnalbuphine for treatment ofintrathecal-morphme-mduced
pruntus in Thai female par-tunents undergoing cesarean section
Design Randomized, double-blind controlled trial Setting- King Chulalongkom Memorial Hospital,
which is the tertiary care center.
Participants Ninety partunents who developed moderate to severe pruntus caused by mtrathecal
administration of morphine after cesarean section were recruited
Interventions The study partunents were randomly allocated into three groups while group
I, II and III received 2, 3 and 4 mg of intravenous nalbuphme respectively
Main Outcome Measure(s) The improvement of pruntus scores and adverse effects ofnalbuphine
(increasing pain scores, nausea and/or vomiting, sedation and respiratory depression) were evaluated
at 5 minutes after nalbuphme administration Results Percentage of successful treatment of moderate
to severe pruntus with 2 mg, 3 mg and 4 mg nalbuphme were 86 7, 96 7 and 100 respectively (p =
0 064) There was also no statistically significant difference in nausea, vomiting and sedation
scores No evidence of respiratory depression was detected in either group However, there was significant
increase in pain scores in group III (4 mg ofnalbuphine) when compared with the other two groups
(p = 0 003)
Conclusions Nalbuphine of 2 to 3 milligrams was considered to be adequate in treatment
of the intrathecal-morphine-induced pruntus after cesarean section since it satisfactorily improved
the symptom without increasing the pain scores or causing other side effects
COMPARISON OF PREEMPTIVE ANALGESIA AND POSTOPERATIVE ANALGESIC EFFECTS OF INTRAARTICULAR MORPHINE
AND KETOROLAC FOLLOWING ARTHROSCOPIC KNEE SURGERY
Sae Jin Choi. Jung Un Lee, Yoon Hee Kirn, Dept ofAnesthesiol-ogy, Chungnam National Univ, Taejeon,
Korea
Aim of Investigation This study was designed to determine the analgesic effect ofintraarticular
morphine and ketorolac combination and whether preemptive analgesic effect of morphine following
arthroscopic knee surgery would present
Methods Thirty patients under regional anesthesia were randomly selected for one of the three
groups Patients in group one (n=10) received 20 ml of saline as placebo, patients in group two (n=10)
received 2 mg of morphine and 30 mg of ketorolac diluted to a total 20 ml with saline; whereas those in
group three (n=10) received 1 mg of morphine before surgery and 1 mg of morphine with 30 mg of ketorolac
diluted to a total 20 ml with saline All the drugs were injected intra-articularly at the conclusion of
arthroscopic procedure and the tourniquet was deflated 10 mm after the injection Postoperative pain was
assessed using visual analogue scale (VAS) at 1, 2, 6, 12, 24 and 36 hr after study drug administration.
The need for supplemental non-narcotic analgesic and side effects of drugs were also noted
Results There were no significant differences among groups with patient characteristics The
most common procedure was partial or complete menisectomy over 70% of the patients The combination of
morphine and ketorolac resulted in decreased postoperative pain and need for postoperative analgesics
And preemptive analgesia with morphine 1 mg mtraarticular injection
Conclusions: Intraarticular injection of the combination of morphine 2 mg and ketorolac
30 mg improves comfort in patients undergoing knee arthroscopic menisectomy
ORAL CONTROLLED-RELEASE (CR) OXYCODONE FOR POSTOPERATIVE PAIN MANAGEMENT
Brian Gmsberg. Duke Univ Medical Center, Durham, NC 27710, Laun Adier*, Magee-Womens Hospital,
Pittsburgh, PA 15213, Michael Ashbum, Univ of Utah Health Sciences Center, Salt Lake City, UT
84132; James Crews, Univ of Cincinnati College of Medicine, Cincinnati, OH 45267-0531, Alien Hord,
Emory Univ Hospital, Atlanta, GA 30322, Charles Launto*, Univ of Illinois Hospital, Chicago, IL
60612-7239, Raymond Smatra, Yale Univ School of Medicine, New Haven, CT 06520-8051; USA
Aim of Investigation To evaluate the safety and effectiveness of CR oxycodone in postoperative
pain.
Methods: More than 12 hr after elective surgery, patients were converted from intravenous
opioids to open-label, oral CR oxycodone (OxyContm®) every 12 hr for up to 7 days 189 patients
who could tolerate oral medications and showed no signs of paralytic ileus participated
Results Mean conversion factors were 1 2 for morphine (n=159), 0 2 for mependme (n=13),
7 3 for hydromorphone (n=10), and 234 for fentanyl (n=6). The most common adverse events, regardless
of causal relationship to study medication, were constipation (25%), nausea (25%), pruntus (16%),
and fever (14%) Paralytic ileus (3%) was the most clinically significant adverse event
| CR Oxycodone Daily Dose and Pain Intensity |
| Study |
|
Daily |
Pain Intensity at |
| Day |
N |
Dose (mg) |
6h Post AM Dose |
| Base |
189 |
— |
4.2 (0.2) |
| 1 |
145 |
56(3) |
3.3 (0.2) |
| 2 |
118 |
52(4) |
3.2 (0.2) |
| 3 |
112 |
44(3) |
3.0 (0.2) |
| 4 |
91 |
39(3) |
3.0 (0.2) |
| 5 |
83 |
37(4) |
2.9 (0.2) |
| 6 |
70 |
31(2) |
3.3 (0.3) |
| 7 |
51 |
27(3) |
2.8 (0.3) |
0=no pain to 10=worst possible pain
Baseline, immediately before initial CR dose.
Conclusions CR oxycodone was an effective analgesic for the oral management of postoperative
pain, and was well tolerated when given after 12 hr postoperatively
Acknowledgments Study sponsor-Purdue Pharma L P
SAFETY AND EFFICACY OF CONTINUOUS INTRAVENOUS OPIOID INFUSIONS VERSUS PATIENT CONTROLLED ANALGESIA
ON GENERAL SURGICAL WARDS: A REVIEW OF 2100 PATIENTS
June Gomnge*. Michael Veltman*, (SPON J Akers), Acute Pain Service, Royal Perth Hospital, Wellington
St Perth, Western Australia, 6000, Australia
Aim of Investigation To determine whether nurse controlled intravenous opioid infusions are
as safe as patient controlled analgesia, when used on general surgical wards in a hospital with an Acute
Pain Service
Methods An observational study was used to analyse the prospective data collected on daily
ward rounds by the Royal Perth Hospital Acute Pain Service. Data from 2,100 patients was analysed
during the study period from May 1997 to October 1998, including 1344 with PCA and 766 with IV
Opioid infusions The ASA of the two groups was compared, along with side effects and quality of
analgesia
Results The ASA of the IV infusion group was higher than the PCA group, with 56% being
ASA 3 or greater, compared to 27% in the latter The frequency and severity of side effects was
similar between groups There were no major complications in either group Pain scores were similar,
while patient satisfaction was slightly higher in the PCA group
Conclusions There is a perception that it is unsafe to run IV Opioid infusions in areas
without access to highly skilled staff and close monitoring facilities We have shown that despite
the IV infusion group having a higher ASA status, it is possible for continuous intravenous opioid
infusions to be run safely and effectively on general surgical wards in a hospital with an Acute
Pain Service
REMIFENTANIL - FIRST CHOICE FOR HIGH-AGED, HIGH-RISK PATIENTS?
Lorenz IH. Kolbitsch C*, Kathrem A*, Luger TJ, Dept of Anaesthesia and Intensive Care Medicine, Dept
of Trauma Surgery, Univ of Innsbruck, Austria
Introduction Remifentanil (Remi), a novel opioid, unique in respect to rapid onset and
offset of its effect Clinical experience with remi for dose regimens and recovery times in patients
being both high-aged (>80 years) and at high-nsk (ASA III-IV) is limited
Case report Use ofremi for mtra- and postoperative analgesia in two high-aged (81 and 84 years;
ASA III-IV), coronary-nsk patients, undergoing major surgery with high blood and fluid turnover rates
Intraoperative monitoring included cardiac output, radial, central venous, pulmonary artenal pressure
Maintenance of anesthesia Isoflurane (0 4%MAC) in 02/Air and infusion ofremi-fentanil (0 17-0 52 m.g
kg ' mm ') A ) 84-year white male presented for acetabuloplasty and total hip arthroplasty after a pelvic
and femur-neck fracture. Medical records showed, aortocoronary graft, aortic valve replacement, impaired
renal function, moderate COPD aggravated by a trauma-related moderate lung contusion B ) 81-year white
male emergency patient for dorsal spine fusion (L3-S1) by starting paralysis of both legs. Medical records.
Myo-cardial infarction, pulmonary embolism, elevated liver enzymes, hepatitis B infection, impaired renal
function Echocardiograph showed reduced left ventncular output, posterolateral akmesia in combination
with aortic valve stenosis.
Results Hemodynamic and pulmonary stability as seen from cardiac index, oxygen delivery,
oxygen consumption, heart rate and MAP were present during induction, maintenance, and in postoperative
care, despite a more than five-hour operation and a total blood and fluid replacement of about
9 L Spontaneous breathing 4 mm after reducing the remi-mfusion, after 10 mm patients were alert
and responsive, so a rough clinical examination of motor function and sensitivity could be performed.
Following mobilization on day 2, discharge to home about 10 days later.
Conclusion Despite the high age and the comorbidity in both cases, a dosage regimen, ignoring
the recommended dose reductions for this age and risk group proved clinically favorable for excellent
hemodynamic and pulmonary stability as well as for rapid recovery from anesthesia and, consequently
early mobilisation on the ward
ANALGESIC EFFICACY OF THE ASSOCIATION D-PROPOXYPHENE - METAMPYRONE IN THE POSTOPERATIVE OF
ABDOMINAL AND GYNECOLOGICAL SURGERY
J M Alvear. C Noboa, D Rodnguez M , V Rodnguez M , G Rentena and the Study Group ofICS-Ecuador, P 0
Box 17-11-6202, Quito - Ecuador E-mail: Jmalvear@accessinter.net
Aim of Investigation We evaluate the efficacy of the association d-propoxyphene/metampyrone
(D/M) for the postoperative treatment of pain in 90 patients that underwent abdominal or gyneco-logical
surgery All of them received every 6 hour 5 cc I V of D/M (50/1500 mg)
Methods: The pain intensity was evaluated using the "visual analogue scale"
(VAS) before the first dose and at: 1, 2, 3, 4, 8, 12, 18, 24, 36 and 48 hours from the beginning
If the pain was VAS > 3, in intensity, another "complementary " dose of the association
D/M (15/450 mg) was given. Pain's intensity progression (X ^ DE) was between 5 55 ± 1 55 (base
line) and 0 25 ± 0 2 at 48 hours Every determination was of significance among themselves (p <
0 05)
Results 24 patients (26 6%) needed one or two complementary doses in order to reach <
3 VAS Adverse reactions were light and observed in 18 patients (20%). One patient presented a
mild allergic reaction. There is not significative statistic correlation between pain intensity
and type of pathology or time of surgical procedure nor with patients age
Conclusions. We conclude that the association D/M offers quick and effective analgesia
in patients undergoing abdominal or gyne-cological surgery and very few side effects
PHARMACOKINETIC STUDY AND POSTOPERATIVE ANALGESIA OF EPIDURAL ADMINISTERED BUPRENORPHINE WTH TWO
DIFFERENT DOSAGES
Yasuko Miwa*. Nonko Shibuya*, Takako Komiyama* (SPON Kazuaki Fukushima), Dept of Anesthesia,
The Kitasato Inst Hospital, and School of Pharmacy, Kitasato Univ, Tokyo, 108-8642 Japan
Aim of Investigation: This study was designed to evaluate the effect of postoperative
analgesia of preemptive epidural administration ofbuprenorphme (BPN) in pharmacokmetic aspects
Method Following approval of institutional ethical committee, 12 patients undergoing surgery
were divided into two groups 5 patients in group-A received 4 ug/kg BPN with 1%, 5ml mepivacame
and 7 patients in group-B received 8 ug/kg BPN with 1%, 5ml mepivacame by epidural route 10 minutes
before the incision respectively The serum concentration of BPN was determined by high performance
liquid chromatography at contro, 5, 10, 30, 60, 180 and 300 minutes. The pharmacokmetic parameters
were examined by nonlinear regression analysis with two-compartment method Postoperative analgesia
was assessed by the dosage of pentazocme required for postoperative pain relief for 48 hours and
by recording VAS scores
Result The peak serum concentration was 2 28 ± 1 34 (mean ± SD) ng/ml in group-A, and
7 75 ± 2 22 ng/ml in group-B. The time to peak concentration was within 5 minutes in both groups
BPN in serum concentration and AUC demonstrated with dose dependent manner Two patients of abdominal
surgery and one patient ofor-thopedic surgery in group-A required pentazocme for postoperative
pain relief None of patients requested pentazocme in group-B postoperatively The VAS score were
under 4 in all patients, but there were remarkable reduced scores in group-B
Conclusions: Epidural administered BPN preemptively transfers quickly into the systemic
circulation and analgesia is secured postoperatively The serum concentration of BPN could be a
good indicator to determine the minimum effective dosage
FENTANYL IMPROVES THORACIC EPIDURAL ANALGESIA PRODUCED BY A LOW-DOSE INFUSION OF BUPIVACAINE, FENTANYL
AND ADRENALINE AFTER MAJOR SURGERY - A RANDOMISED, DOUBLE-BLIND CROSS-OVER STUDY WITH AND WITHOUT FENTANYL
Geir Niemi and Harald Breivik, Dept of Anaesthesiology, The National Hospital (Rikshospitalet), N-0027
Oslo, Norway.
Aim of Investigation To evaluate the effects on postoperative pain intensity, pain relief
and side effects when removing fentanyl from an epidural mixture consisting ofbupivacame, fentanyl
and adrenaline
Methods A prospective, randomised, double-blind, cross-over study was earned out in 20 patients
after major abdominal surgery Patients with only mild pain when coughing during thoracic epidural infusion
of about 10 ml per hour ofbupivacame 1 mg ml , fentanyl 2 m.g ml ', and adrenaline
2 mg ml ' were included On the 1st and 2nd postoperative
day each patient was given a double-blind epidural infusion, at the same rate, with or without fentanyl
The effect was observed for 6 hours or until pain when coughing became unacceptable in spite of rescue
analgesia Rescue analgesia was up to two patient controlled epidural bolus injections (4-ml) per hour
and intravenous morphine if necessary All patients received rectal paracetamol 1 g, every 6 hours. Main
outcome measures were pam intensity at rest and when coughing
Results. The pain intensity at rest and when coughing increased (p<0 001) when fentanyl
was omitted. This change started within three hours after removing fentanyl After 6 hours pain
intensity when coughing had increased to unacceptable levels in spite of rescue analgesia. Within
15-20 minutes after restarting the triple epidural mixture with fentanyl, pain intensity was again
reduced to mild pain when coughing
Conclusions Fentanyl improves the pain relieving effect of a mixture ofbupivacame and
adrenaline infused epidurally at a thoracic level after major abdominal surgery
INTRATHECAL MIDAZOLAM AND BUPRENORPHINE: A COMBINATION FOR POSTOPERATIVE PAIN RELIEF
Baheti O.K.. Par Dhungat P P *, Dept of Anesthesiology, Bombay Hospital Inst of Medical Sciences, 12,
New Manne Lines, Mumbal 400 020 INDIA
Aims of Investigation To find out the efficacy of combination of mtrathecal Midazolam and Buprenorphme
for postoperative pain relief
Methods All patients received Midazolam 2mgm (preservative free) initially and then Buprenorphme
0 15mg, along with Bupiva-caine was injected intrathecally The degree and duration of postoperative
pain relief was assessed by visual analogue scale, respiratory rate, heart rate and blood pressure
were monitored In postoperative penod Inj Ketonov mtramuscularly as and when required However
in gynecological operations Inj Ketonov was given at six hours and eighteen hours to prevent movement
pain
Results Sixty patients of A S.A I & II undergoing general surgical, urological and
gynecological operations were included In 50% (n=30) no analgesic was required even after thirty-six
hours In gynecological operations (n=30) cases twenty patients did not require analgesic whereas
remaining ten patients required Inj Ketonov after twenty-four hours Two patients, of abdominal
hysterectomy, had nausea and vomiting, which was controlled with Inj Ondansetron The pain relief
score varied between 1 & 2 and other parameters were within normal limits All the patients
had good pain relief up to 18-24 hours and had no pain at the incision site No patient required
sedation either during or after surgery
Conclusions We conclude that mtrathecal Midazolam 2mgm and Buprenorphme 0 15mg is a useful combination
for postoperative pain relief The pain relief was for eighteen hours or more None of the patient required
any sedation during and after surgery
ORAL TRAMADOL IS AS EFFECTIVE AS INTRAMUSCULAR MORPHINE FOR PAIN RELIEF AFTER INGUINAL HERNIA
SURGERY
A Numanoglu*. P A Goldberg, (SPON EA Shipton), A NicoF, D Folscher , E Thomas**, MFJ James"*,
Depts of Surgery* and Anaesthetics*, Univ of Cape Town and Groote Schuur Hospital, Observatory Cape Town
7925 South Africa
Aim: The availability of an effective, safe and well tolerated oral analgesic in the early
post-operative penod after inguinal surgery would be an advantage Tramadol, a partial opioid agonist,
with limited opioid-type side effects, might fulfil these criteria We have compared the analgesic
efficiency of oral tramadol with intramuscular morphine in a prospective double blind randomized
trial
Patients and Methods. Eighty-six fit male patients (median age 47, ql-q3 30-57) undergoing
unilateral inguinal hernia surgery were randomised to receive either tramadol or morphine (43
in each group). Patient controlled analgesia (PCA) loaded with morphine (1.5 mg /dose, 8 minute
lockout time) was used as rescue analgesia in all patients During the first 24 hours after operation,
patients randomised to receive tramadol were given 3 mg/kg intravenous tramadol with induction
of anaesthesia, and post-operatively, capsules containing 2 mg/kg tramadol 6 hourly and placebo
injections of normal saline (0.01 ml/kg) Patients randomised to receive morphine were given 0.15
mg/kg intravenous morphine with induction, 0.15 mg/kg morphine injections 6 hourly and placebo
capsules by mouth
Results. Complete data was available for analysis in 68 patients (32 randomised to tramadol,
36 to morphine). The 2 groups were well matched in age, body weight, and type ofhemia repaired.
There was no statistical difference between the two groups in the total amount of morphine delivered
by the PCA machines (tramadol median 12 0 mg (ql-q3 9-18) v morphine 13 5 mg (6-23 5)) (p=0.66)
or in the number of unsuccessful demands (tramadol median 2 5 (ql-q3 0-4 5) v morphine median
3 5 (ql-q3 1-9 75)) (p=0 3) The number and type of side effects recorded were similar Both the
absolute and percentage fall in systolic blood pressure at 5 and 10 minutes after induction of
anaesthesia was significantly greater in the control group (p<0 05)
Conclusion Oral tramadol (2 mg/kg) provides similar postoperative analgesia to intramuscular
morphine (0 15 mg/kg) Tramadol causes significantly less hypotension after induction of anaesthetics
POSTOPERATIVE ANALGESIA WITH OXYCONTIN FOLLOWING AMBULATORY ACL REPAIR SURGERY
SS Reuben. NR Connelly*, CS Gibson*, H Macioiek*, Baystate Medical Center and the Tufts Univ
School of Medicine, Dept of Anesthesia, Springfield, MA 01199, USA
Aim of Investigation To determine whether a controlled-release formulation ofoxycodone (OxyContin®)
is more clinically acceptable than immediate-release oxycodone in the management of pain following ambulatory
ACL repair surgery
Methods 60 patients undergoing ambulatory ACL surgery received a standard general anesthetic
with propofol, fentanyl (2 ug/kg), ketorolac, and mtraarticular bupivacame and morphine All patients
received postoperative cryotherapy and were randomized to receive either 1 of 3 analgesic regimens
Group 1 were instructed to take oxycodone 5mg 1 -2 tabs q 4h pm pain Group 2 were instructed to
take oxycodone 5mg 2 tabs q 4h with 1 tab q 6h pm breakthrough pain Group 3 were instructed to
take OxyCon-tm® 20 mg q 12h with oxycodone 5mg 1 tab q 6h pm breakthrough pain Patients recorded
their pain (0-10) and degree of sedation every 12h They were also asked to record their sleep
disturbance for the first 3 nights after surgery Side effects such as nausea, vomiting, and pruntus,
were also recorded At the completion of the study (72h), patients rated their satisfaction with
their pain medicine
Results There were no differences among the groups in demographic vanables or duration
of surgery Total oxycodone use (mg) in 72h was significantly lower (p< 00 1) in group 3 (123±4)
compared to group 2 (16U13) or group 1 (139±17) Patients in group 3 had significantly lower pain
and sedation scores (p< 0 0001), were more satisfied (p< 001), and experienced less vomiting
(p< 0 02) compared to the other two groups
Conclusions The use of controlled-release oxycodone in the immediate 72 hours following
ambulatory ACL surgery provides more effective analgesia, with less sedation, sleep disturbance,
and postoperative vomiting, when compared to oxycodone prescribed on either a fixed dose or as
needed schedule
PERIPHERAL MORPHINE ANALGESIA IN DENTAL SURGERY PATIENTS
M Schafer. R Likar, C Stem, Deps ofAnesthesiology,Freie Universitat Berlin/Germany, and Klagen
furl/Austria
Aim of Investigation To examine in a unique clinical model of inflammatory tooth pain
the analgesic efficacy of local morphine treatment applied to inflamed, non-inflamed and penneural
tissue
Methods Patients undergoing dental surgery were randomly assigned to an injection of local
anesthetic (articame) plus 1 mg morphine either into inflamed (n=22) or non-inflamed (n=26) sub-mucous
tissue or penneurally (n=27) Patients in the control group for each condition (n=22, n=25, n=27,
respectively) received arti-came plus saline Postoperative pain intensity was assessed by the
Visual Analog Scale (VAS) and Numeric Rating Scale at 2, 4, 6, 8, 10, 12, 16, 20, and 24 h In
addition, patients recorded the occurrence of side effects and the supplemental consumption ofdiclo-fenac
Results. Pain scores were reduced to a similar extent in all groups up to 6 h postoperatively
due to the local anesthetic effect Thereafter, pain scores and the supplemental consumption ofdiclofenac
were significantly lower in patients receiving 1 mg morphine into inflamed submucous tissue than
in the control group for up to 24 h (P < 0 05, ANOVA) Patients receiving 1 mg morphine into
non-inflamed tissue or penneurally did not show any further reduction in pain scores
Conclusions Our results show in patients undergoing dental surgery that injection of 1
mg of morphine into inflamed tissue results in significant and prolonged postoperative analgesia,
whereas administration into non-inflamed tissue and penneurally is not effective Thus, the requirement
of an inflammatory process for the occurrence of peripheral opioid effects is also found in the
clinical setting
SAFETY AND EFFICACY OF SUSTAINED-RELEASE ENCAPSULATED MORPHINE (C0401) FOR POSTOPERATIVE
ANALGESIA
ER Viscusi. MC Toyman*, DJ Correll*, TA Witkowski*, R Jan*, JB Lessin*, AT Marr*, M Schrmdt*
Dept ofAnesthesiology, Jefferson Medical College, Thomas Jefferson Univ, Philadelphia, PA 19107
USA
Aim of Investigation In order to extend the duration of analgesia but eliminate the need
for continuous epidural catheters a new lipid-based mjectable drug delivery system, DepoFoam™
(Depo-Tech Corp , San Diego, CA), was used to encapsulate morphine (C0401) In this ongoing Phase
II open label study we wished to determine the safety and efficacy of C0401 administered epidurally
for treatment of postoperative pain in patients undergoing total hip arthroplasty (THA)
Methods Following IRB approval, informed consent was obtained from patients presenting
for THA A 20mg dose of C0401 was injected over 15 seconds via the epidural Postoperatively patients
had access to a fentanyl PCA for 48 hours and acetammophen with codeine thereafter for additional
pain control as needed Patients were assessed for 72 hours for pain (100mm VAS scale), adverse
events and side effects
Results The mean time to first use of rescue analgesic was 37 9 hours and ranged from
17 to 52 5 hours in four patients One patient required no supplemental analgesic during her entire
hospital course Four of the patients had nausea/vomiting during the first 24 hour penod that was
effectively treated pharmacologically After the first 24 hours one patient expenenced mild nausea
not requiring therapy All patients expenenced pruntus dunng the first 24 hours The lowest RR and
SpO^ values recorded were 8 breaths/mm and 94% respectively Those occurred postoperatively within
the first 8 hr post C0401 dose
Conclusions. Based upon these preliminary data, the duration and quality of analgesia
from a single epidural injection of C0401 is far superior to a single dose of either intrathecal
or epidural morphine in this population The side effect profile is similar to that seen with standard
opioid therapy and in most cases was easily treated
Acknowledgments Supported by DepoTech Corporation, San Diego, California USA
AN ASSESSMENT OF THE INFLUENCE OF PRE-OR INTRAOPERATIONAL USE OF TRAMADOL (PREEMPTIVE OR PREVENTIVE
ANALGESIA) ON OPIOID REQUIREMENT IN THE EARLY POSTOPERATIVE PERIOD
J Wordhczek. T Krzyzanowska*, T Cleniawa*, M Banach*, W Serednicki*, H Wiatrak*, I Grabowska*,
J Gariicki*, J Dobro-gowski, Dept of Pain Research and Treatment, Collegium Medi-cum Jagiellonian
Univ, ul Sniadeckich 11, 30-531 Krakow, Poland
Aim of Investigation was to assess the influence of i v tramadol administered before general
anaesthesia (N2O/O2 + isoflurane), immediately after pentoneal closure, or immediately after operation,
on opioid requirement in the early postoperative penod
Matenal and Method. Investigated were 90 patients scheduled for colon surgery 30 patients
(I group), were administered 100 mg of tramadol i v before induction (preemptive analgesia) Next
30 patients (II group), were administered 100 mg of tramadol i v immediately after pentoneal closure
(preventive analgesia) The III group (30 patients) received 100 mg of tramadol i v immediately
after operation After the operation all patients were administered tramadol in the PCA-i v mode
in order to treat postoperative pain In the postoperative penod the following parameters were
measured pain level (using VAS), total consumption of tramadol, time until the first PCA activation,
and frequency of side effects (drowsmess, nausea, vomiting)
Results In group I and II (preemptive or preventive analgesia) observed was a significantly
lower total consumption of tramadol as compared with group III However, the time until the first
PCA activation was significantly shorter in group I No significant differences between the groups
were found regarding pain intensity and frequency of side effects
Conclusions. Pre- or mtra-operational use of tramadol (preemptive or preventive analgesia)
significantly reduces opioid requirement in the early postoperative penod
Acknowledgments. Supported by grant WL/241/KL/L Coil Med Jagiellonian Univ and Grunenthal GmbH
ANALGESIC REQUIREMENTS LIVING RELATED KIDNEY DONORS
Altintas F, Bozkurt P, Kaya G, Kose Y, I U Cerrahpasa Medical Faculty, Dept of Anesthesiology, Istanbul,
Turkey
Aim of Investigation This study is undertaken to evaluate the analgesic requirements of
donor nephrectomies versus nephrectomies earned out for urological reasons
Matenals and Methods Twenty-seven healthy patients undergoing donor nephrectomy (Group
I) (male/female 7/20), age 52 6±11 5 years) and 16 patients with several self pathologies undergoing
nephrectomy (Group II) (male/female 5/11, age 42 3± 14 6 years) in lateral decubitus position
were included in this study following consent of the patients Patients have been informed bout
patient control analgesia (PCA) and verbal analogue score (VAS) for pain assessment was defined
A standardized general anesthesia method used for all patients Morphine 0 15 mg/kg was injected
subcutane-ously before the commencement oflombotomy closure PCA initiated which was programmed
as bolus 2 mg morphine sulfate (morphine in 1 mg/ml of 100 ml isotonic saline), lockout time 8
minutes, 4 hour limit 40 mcg/kg by the attendant anesthesiologist Heart rate, systolic blood pressures,
respiratory rate, SpO; VAS scores and side effects were recorded every 2 hours for 24 hours The
amount of drug delivered, demands of the patient were recorded from the history of the PCA Fisher's
exact test and student t-test were used for statistical analysis
Results No vital changes observed in cardiorespiratory parameters in both groups VAS varied
from 0 to 8, median 5 in Group I and from 0 to 5, median 3 in Group II The amounts of delivered
morphine were 42 1±19 1 mg and 35±9 79 mg Group I and II in 24 hours, respectively (p<0 05)
Group I had demanded for morphine 85 4±63 0 times and Group II 34 8±29 6 times (p<0 05)
Conclusion- Differences in demands and the amounts of delivered analgesic between two
groups might be related to the different expectations of the patients in each group
TRAMADOL HYDROCHLORIDE (TRAMAL) VERSUS MORPHINE FOR POSTOPERATIVE PAIN RELIEF
Enaam Fouad Gadalla. Professor of Anaesthesia, Benha Faculty of Medicine, P 0 Box 144 Benha Egypt
Aim of Investigation To compare the clinical efficacy of tramadol with that of morphine
in postoperative pain relief
Methods Sixty middle-aged patients subjected to lower abdominal and lower limb surgeries
under genera] anaesthesia were the subject of this study They were divided into two equal groups
After recovery of the patients and when they first complained of pain, they were given the analgesic
drug in a bolus dose mtravenously Patients of group I were given tramadol (100 mg) while patients
of ;roup II were given morphine sulphate (10 mg). Top-up doses of he analgesic were given to responders
on demand in the form of SO mg tramadol or 5 mg morphine intravenously in the first 24 lours.
Efficacy of the analgesic drug using verbal rating scale was :valuated and compared in the two
groups as well as incidence and requency of side effects of the drugs in each group.
Results: Responders (after 90 min.) of the tramadol group were )0% of the patient while
they were 95% of the patients in the mor-ihine group. Onset of action of the drugs was rapid in
both groups with a mean value of 13 minutes in the tramadol group and 10 min. n the morphine group.
The time between the 1st and 2nd doses of :ramadol and morphine was comparable
in both groups as well as :he intervals between all subsequent doses in both groups. Mean values
of total dose of the drugs over the first 24 hours period was 270.2 mg tramadol and 26.5 mg morphine.
Adverse effects were mainly gastrointestinal (nausea and vomiting). They were observed in both
groups with higher incidence in the tramadol group. There ivas more sedation in the morphine group.
Respiratory depression 3ccurred in two patient of morphine group and non in the tramadol group.
Conclusions: The study showed that tramadol is as effective as •norphine for postoperative
analgesia in a dose ratio of 10:1. Tramadol is safer than morphine as a postoperative analgesic
as it ioes not cause respiratory depression.
A COMPARISON OF NURSE-ADMINISTERED TRAMADOL AND PATIENT-CONTROLLED ANALGESIA OF THE SAME
DRUG
N.H. Adib, Dept of Anesthesia and Pain Clinic, AL- Saydeh Hospital Damascus, Syria.
Aim of Investigation: This study compared the efficacy of Tramadol hydrochloride administered
by patient-controlled analgesia (PCA) with intermittent intramuscular injection (IMI) for post
operative pain control.
Methods: Patient undergoing abdominal gynecological surgery (n=184) were randomly allocated
to one of 3 treatment groups receiving Tramadol for postoperative pain control: Group 1, PCA (lOmg
demand with a 2 min. Lockout interval plus 15 mg^ mandatory infusion) and group 2 and 3, IMI (100
mg, PRN up to every 2h). Categorical seals were used to measure pain, nausea, sedation and sweating
in groups 1 and 2 every hour for the first 24h; group 3 had routine postoperative observation.
On the day after surgery patients were asked to complete a questionnaire on their postoperative
pain relief. Three weeks later another questionnaire on pain control was sent to all patients.
Results: Patients using PCA received significantly (p<0.0001) more Tramadol (mean 548
mg/24h) than was administered by nursing staff to the IMI groups (mean 395 mg/24h) and had 30%/mean)
more tramadol than those in group 3, but in the 24h questionnaire they recalled worse pain relief.
In the post discharge questionnaire groups 2 and 3 recalled similar (mean) pain scores which were
worse than in group 1.
Conclusions: Judged by patients' reports of pain, PCA provided better pain relief than IMI due,
in part, to that group receiving more tramadol. Although hourly measurement of postoperative pain
during IMI led to nursing staff administering more Tramadol to those patients, the corollary in
that group was not less pain.
PATIENT CONTROLLED ANALGESIA (PCA) WITH FAST TRACK CORONARY ARTERY BYPASS (CABG) PATIENTS
Yvonne D'Arcy* (SPON: Jerry Hall), Dep ofAnesthesiology, Mayo Clinic Jacksonville, Jacksonville
FL. USA
Aim of Investigation: To examine the use of PCA as a means of pain control in the ICU
with post-operative cardiac surgery patients.
Methods: A convenience sample of 14 patients who had undergone cardiac surgery was interviewed
before discharge for recall of pain experiences while in ICU. Chart review was done on these patients
for pain score documentation and medication usage while in ICU.
Results: 50% of the patients had clear recall of painful events while in the ICU. Painful
areas were: chest tubes and pacer wires, ventilator discomfort, chronic pain conditions, and distress
at limited communication related to ventilation. 9 of the 14 patients had either morphine or meperidine
PCAs. Morphine usage ranged from 3.0 to 217.0 mg during the ICU stay, meperidine 136.0 to 215.0
mg. Pain rating average for all patients was 5.8 on the VAS pain scale. The PCA group had a pain
scale rating average of 3.9 on the VAS, while the non-PCA group had an average of 8.8. Three patients
were maintained solely on propofol drips with no pain medications and had the highest pain scores
in the group.
Conclusions: Interviewing the cardiac patients provided evidence that PCA was useful in
decreasing pain in post CABG patients. Chart review indicated that clarification of sedation versus
pain medication was needed as well as emphasis on the importance of adequate pain management in
the immediate post-operative setting.
A COMPARISON OF PATIENT-CONTROLLED EPIDURAL PETHIDINE VERSUS SINGLE DOSE EPIDURAL MORPHINE FOR
ANALGESIA POST CAESAREAN SECTION
M.P. Fanshawe*. (SPON: B. Williams), Dept ofAnaesthesiology & Intensive Care, Redcliffe Hospital,
Redcliffe, Queensland, 4020, AUSTRALIA
Aim of Investigation: This double-blind, randomised study compared patient controlled
epidural analgesia (PCEA) with pethidine versus single dose epidural morphine.
Methods: Eighty-seven patients were enrolled. Group P received epidural pethidine 50mg
upon delivery and a pethidine PCEA (15mg of a 0.25% solution and a ten minute lockout). Group
M received 4mg of epidural morphine and a normal saline PCEA. Visual analogue scores were collected
for analgesia, nauseaV vomiting, and itch at two, six, eight, and twenty-four hours post-caesarean.
A multinomial logistic regression model was used to assess the full range of scores and the scores
at each time. Results: There was no difference in pain (p=0.78) and nausea/ vomiting (p=0.185)
for the full range of scores. Time specific pain scores were higher for Group M at two hours (p=0.004)
and higher for Group P at six hours (p=0.003). Time specific nausea scores were higher for Group
M at six and eight hours (p=0.024). Itch was lower in Group P for both the full range of scores
and at all time points (p<0.001). Group P used 192+/-42mg and Group M 38+/-29mls (SEM).
Conclusion: Single dose epidural morphine is commonly used post caesarean. Epidural pethidine
is pharmacokinetically suitable for PCEA usage. The results show that PCEA pethidine causes less
itch. Whether less itch is worth the time, machinery, and higher systemic opiate levels compared
with single dose morphine is debatable. Certainly in patients with a contra-indication to epidural
morphine, PCEA pethidine provides a useful alternative for the provision of analgesia post caesarean.
Acknowledgments: Redcliffe/Caboolture Hospitals
SICKLE CELL DISEASE (SCD) PATIENTS' PERCEPTIONS OF PATIENT CONTROLLED ANALGESIA (PCA)
Lucy Johnson* (SPON: F. D'Costa), Pain Relief Unit, King's College Hospital, London SE5 9RS,
UK. Aim of Investigation: To study patients' perceptions of self-administering diamorphine subcutaneously
via an electronic infusion pump.
Methods: All adult SCD patients hospitalised between April and July 1998 deemed fit enough
to participate were offered a previously-piloted questionnaire comprising open-ended and multiple-choice
questions. Following initial analysis of results, five respondents voluntarily contributed to
a focus-group discussion probing key issues raised
Results From 44 patients admitted, 18 males and 22 females responded Aged 18 to 49 years,
all had expenence ofopioids for acute pain and two-thirds had used diamorphme PCA Independent
of gender, age and previous opioid-expenence, they agreed strongly in their views about PCA's
main potential attractions timely pain relief (80%) and freedom from staff (80%) They identified
bamers to PCA's more widespread acceptance' ineffective analgesic regimens, poor mechanical reliability
and portability, cannula problems and reduced nursing intervention. Inter alia, they rated pethidme
as marginally the most effective analgesia but dia-morphme as most desirable because of more tolerable
side-effects
Conclusions Severe pain is the overriding manifestation ofSCD, one of the world's most
common hereditary disorders, and its impact can be profoundly disabling The contemporary view
is that SCD pain is best controlled by patients themselves because there are no objective signs
early in acute episodes and pain assessment is essentially subjective The study's patient-data
broadly support this view It affirms, for the first time, SCD patients' backing for diamorphme
PCA's usage It provides recommendations for increasing the modality's acceptance covering improvements
in technical design, training and patient-staff communication
PREDICTORS OF SATISFACTION WITH PATIENT-CONTROLLED ANALGESIA FOR THE MANAGEMENT OF POSTOPERATIVE
PAIN
Joel Katz, Lucia Gaghese. Adarose Wowk*, Paul Ritvo*, Maria Jackson*, Alan Sandier, Depts of
Psychology and Anaesthesia, The Toronto Hospital, Toronto, Ontario, M5G 2C4, Canada
Aims of Investigation To identify predictors of satisfaction with patient-controlled analgesia
(PCA) for postoperative pain control
Methods Preoperatively, patients (n=89) were instructed in the use of PCA and completed measures
of psychological distress, desire for behavioural control (BEHAV) and information regarding their health
care, anticipated postoperative pain, attitudes towards PCA, and PCA-related self-efficacy (SE-PCA) Upon
arrival in the recovery room after surgery, patients received a loading dose of demerol or morphine and
were immediately placed on a PCA pump Pain intensity was measured daily using visual analog scale (VAS).
Cumulative opioid intake (ANALG) and total number of days on PCA were recorded Patients completed the
PCA Satisfaction Survey when PCA was discontinued Results Stepwise regression analysis was conducted with
the demographic, preoperative and postoperative measures as potential predictors of satisfaction The best
model identified included a constant, ANALG, BEHAV, SE-PCA and VAS For this model, R =041^=0 17, F (4,
85)= 4,368, p= 0.003.
Conclusions: Satisfaction with PCA can be predicted by psychological factors, pain levels
and analgesic requirements Patients who indicated a greater desire for behavioural control over
their health care and greater confidence in their ability to use PCA effectively subsequently
reported greater satisfaction with PCA Postoperative influences on satisfaction included amount
ofopioid self-administered and pain intensity These results imply that preoperative interventions
that increase self-efficacy and desire for behavioural control over health care may lead to greater
satisfaction with PCA postoperatively
Acknowledgments Supported by MRC Grant MT-12052 and NIH Grant NIH-NS35480.
THE EFFECT OF PRE-OPERATIVE TEACHING ON PATIENT CONTROLLED ANALGESIA USE
K McCormick*. A Forsey, J Kay, R Hargadon*, J Lam-McCulloch*, Dept of Anesthesia, Sunnybrook
& Women's Health Sciences Centre, 2075 Bayview Ave , Toronto, Ontario, M4N 3M5 Canada
Aim of Investigation To evaluate the effect ofpre-operative teaching on post-operative
pain intensity, opioid use, anxiety, satisfaction and understanding of pain management strategies
in patients using patient controlled analgesia (PCA)
Methods 70 patients undergoing elective surgery were randomized to receive, pre-operatively,
either a structured teaching session with a Registered Nurse, or no formal teaching concerning
PCA Pain (VAS), anxiety (Beck Anxiety Inventory - BAI), and knowledge about PCA were evaluated
prior to surgery At 24 hr post-operat-ively, pain scores amount ofopioid use, BAI, satisfaction
score, number of unsuccessful delivery attempts and knowledge of pain management strategies were
collected by a blinded observer At 72 hr post-operatively, a qualitative interview was conducted
to ascertain what information patients found helpful in the teaching session
Results The interim analysis on 70 patients shows that satisfaction was higher in the
group that received pre-operative teaching (p<0 04) There was a trend for less opioid use and
fewer unsuccessful delivery attempts in this group There was no difference in pain scores Patient
feedback indicated a preference for direct contact with a health professional versus video or
handout only Information gaps identified included side effects and latency of the drug effect
Conclusion These preliminary findings indicate that patients receiving a structured interactive
teaching session pre-operatively have higher satisfaction with their pain management This study
is ongoing
TRAINING PROGRAM FOR NURSES FOR THE UTILIZATION OF INFUSION PUMPS FOR PATIENT-CONTROLLED ANALGESIA
Cell Regma Noca*, Lucimara D Chaves, Antonia Raponi*, Dan-lela M dos Santos*, Nimia L Monteiro*,
Gladys Antonioli*, Ro-sana Frazao* Hospital Alemao Oswaldo Cruz, Pain Therapy Service, Rua Joao
Jubao, 331, Paraiso, Sao Paulo, Brasil CEP 01323-903
Aim of Investigation To render all nurses in a private general hospital in Sao Paulo,
Brazil, capable of handling infusion pumps for patient controlled analgesia
Methods Training program prepared by nurses working at the Pain Therapy Service and Continued
Education Service of Hospital Alemao Oswaldo Cruz The program was conducted in four phases 1)
Raising of each hospital nurse's doubts on an individual basis through a specific questionnaire,
2) Application of practical individual training with presentation of simulated situations, based
on the doubts presented by the nurses themselves in the initial questionnaire, 3) After each training
session, assessment through specific printed paper in the form of check-list, 4) Delivery of illustrated
manual demonstrating all the equipment handling Results As a result, it was possible to offer
an individual training on patient-controlled analgesia procedures with the use of infusion pumps,
specifically designed to nurses
Conclusions The evaluation of the results in relation to apprenticeship levels and incidence
of mistakes during the procedure will be presented in August, 1999
PATIENT-CONTROLLED EPIDURAL ANALGESIA (PCEA) IN LABOUR. THE ADDITION OF CLON1DINE TO BUPIVACAINE-FENTANYL
Michael Paech*. Timothy Pavy, Sharon Evans*, Dept of Anaesthesia, K-mg Edward Memorial Hospital,
Subiaco 6008, Perth, Western Australia
Aim of Investigation Epidural clonidme boluses during labour may cause sedation and alter
haemodynamics We wished to determine ifclonidme was useful and free of side effects when included
in a patient-controlled epidural analgesia (PCEA) regimen
Methods A randomised, double-blind controlled trial in 75 healthy partunents, assigned
to PCEA solution ofO 0625% bupivacame and fentanyl 2 mcg/ml (4 ml demand bolus; 15 mm lockout),
with or without clonidine 4.5 mcg/ml.
Results: After 6 exclusions, 31 received clonidine (group BFC) and 38 the control solution
(group BF). Six in group BF and 2 in group BFC failed to achieve satisfactory epidural analgesia
(p = 0.28). Clonidine (median dose 28 mcg/h) reduced total bupivacame and fentanyl use (p <
0.01); lowered the rate of supplementation (p < 0.01) and produced similar pain scores. Analgesia
ratings in both stages of labour were higher in group BFC, significantly more women reporting
excellent first stage analgesia (81% vs 57%, p < 0.05). Maternal blood pressure (BP) and episodes
ofsystolic BP below 100 mmHg did not differ. Group BFC had higher sedation scores (10 units, 0-100
scale; p < 0.01), but these were low in both groups. Shivering was reduced in group BFC (p
< 0.01). Neonatal Apgar scores were similar.
Conclusions: Under the study conditions, the addition of clonidine 4.5 mcg/ml to 0.0625%
bupivacame and fentanyl 2 mcg/ml for PCEA during labor conferred minor benefit and no clinically
important maternal disadvantages.
Acknowledgments: Supported by a grant from the Women and Infants Research Foundation
PATIENT CONTROLLED ANALGESIA VERSUS TRAMADOL PLUS LYSINE ACETYL SALICYLATE
WW Pang*. MH Huang*, MS Mok*, ST Ho, Dept. of Anesthesia, Show-Chwang Memonal Hospital, ChangHua,
Taipel Medical College & Tnservice Gen. Hosp., Taiwan
Aim of Investigation: Using PCA delivery system we evaluated the clinical effect oftramadol
(T) compared to T plus lysme acetyl salicylate (LAS), an mjectable aspinn.
Method: Following major orthopedic surgery under general anesthesia 50 patients were enrolled
into this double-blind, randomized, prospective study. At wound closure a loading dose of either
T 6mg/kg or T 3mg + LAS 27 mg/kg I.V. was given. In the post anesth room equal volume PCA of either
T 30 mg/ml or T 15 mg + LAS 13.5 mg/ml were used with lock out interval of 10 mm to achieve analgesia
with Visual Analog Score (VAS)<4. Pain relief, satisfaction score, vital signs and side effects
were recorded for 48 h.
Results: Adequate analgesia (VAS<4) was achieved with either drug. Tramadol consumption
in the T/LAS group was significantly less than in the T group both at 24 and 48 hr. (p<0.05).
Nausea and sedation were reduced in the T/LAS group. Blood loss was similar between the 2 groups.
Conclusion: Parenteral aspinn could be used as an effective and safe adjuvant to tramadol
for PCA use in the relief of post surgical pain. This combination reduces the dose requirement
oftramadol, hence some of its adverse effects.
PDA VERSUS PCA FOR POSTOPERATIVE PAIN CONTROL: EVALUATION BY THE TYPE OF SURGERY
Robert Reichhalter*. Wolfgang Jaksch, Sylvia Fitzal*, Dept of Anesthesia and Intensive Care,
Wilhelmmenspital, Montleart-strasse 37; A-1171 Vienna, Austria
Aim of Investigation: To analyze the intensity of postoperative pain during lumbar pendural
anesthesia (PDA) or i.v. patient- controlled analgesia (PCA) following different surgical procedures
in a retrospective study.
Methods: To relieve postoperative pain patients received either PDA with ropivacaine 0.2%,
5 - 8 ml/h, or i.v. PCA (Abbott Life-care) with pintramide, 3mg/ml (1.5mg boluses; 8 mm lock out
time; no basal rate; 4-hour max. dose 30mg). Using a 10-score visual analog scale, pain at rest
(VAS-R) and pain at movements (VAS-M) were evaluated dunng the first 3 postoperative days and
related to the type of surgery (abdominal, trauma, vascular, gyne-cologic and urologic).
Results: In 843 patients a total of 3,280 VAS scores were recorded. 299 patients were
on PDA, while 544 received PCA. In patients on PDA both VAS-R and VAS-M scores were significantly
lower than in PCA patients (1.28 and 2.54 versus 1.64 and 3.68). Patients who had undergone abdominal
and trauma surgery benefited most from PDA (VAS-R 1.18 and 1.24 versus VAS-R 1.69 and 1.57 for
PCA), while no method-related differences were seen after urologic, gynecologic and vascular procedures.
VAS-M scores were lower in patients on PDA than those dunng PCA only after abdominal and urologic
surgery (2.24 vs. 3.52 and 3.15 vs. 3.71).
Conclusions: Both pain control regimens proved to be effective with VAS-R scores <
3 and VAS-M scores < 5. Following abdominal and trauma surgery PDA appears to be most beneficial,
whereas postoperative pain following other surgical procedures is equally well relieved by either
procedure.
DOSE FINDING STUDY ON DROPER1DOL AS AN ADJUNCT TO MORPHINE VIA PATIENT-CONTROLLED ANALGESIA
TO REDUCE POST-OPERATIVE NAUSEA AND VOMITING
Q. Shen*, S. A. Schug. J.E. Ritchie*, J.M. Thomas*, D.A. Side-botham* (SPON: J. Bamard), Section
of Anaesthetics, Univ of Auckland, Auckland, New Zealand
Aim of Investigation: To find an effective and safe dose ofdro-pendol as an adjunct to
morphine via patient-controlled analgesia (PCA) as a way of reducing postoperative nausea and
vomiting (PONV).
Methods: One hundred consenting patients requiring PCA after undergoing acute orthopaedic
surgery under general anaesthesia were recruited. In a double-blinded design they were randomised
to use PCA pumps (morphine bolus 1 mg, lock out 5 mm) with pre-filled synnges containing one of
four mixtures: DO - no dropendol added; DO.02 - 0.02 mg dropendol per 1 mg morphine; DO.05 -0.05
mg dropendol per 1 mg morphine; DO.1 - 0.1 mg dropendol per 1 mg morphine. The incidence of PONV,
requests for rescue anti-emetics, and side effects were recorded for up to three days after operation.
Results:
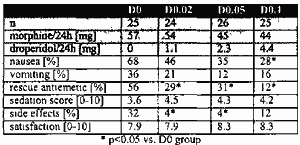
Conclusions: Adding small amounts of dropendol to morphine via a PCA device significantly
reduces the incidence of nausea and vomiting and the requirements for rescue antiemetics in a
dose dependent fashion without increasing side effects. An addition of dropendol 0.05-O.lmg per
1 mg morphine seems a suitable dose.
9th WORLD CONGRESS ON PAIN, 1999, Vienna, Austria, p.71 - 78
|

